Published: 04/24/2026
By Catherine Wu, Global Health Communications Assistant
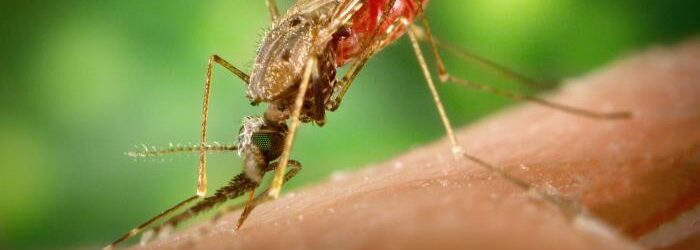
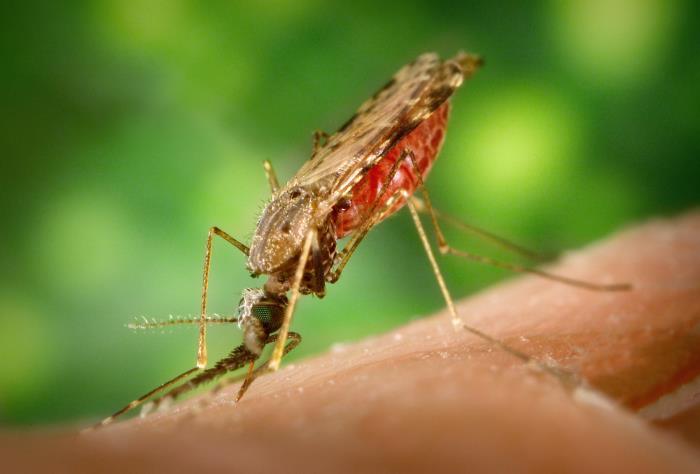
On World Malaria Day, April 25, we recognize global efforts to raise awareness of the life-threatening disease, transmitted to humans through infected female Anopheles mosquitoes.
At Stanford, researchers like Dr. Prasanna Jagannathan, associate professor of infectious diseases, drive studies to better understand malaria. In his lab, Jagannathan studies the human immunology of infectious diseases, including naturally acquired immunity to malaria in childhood.
Jagannathan’s malaria research was inspired by a rotation in Uganda, where he saw firsthand the toll malaria took on communities. He noticed that many children, despite repeated malaria infections, rarely became severely ill.
“What fascinates me, and what inspired my work, is that over time, children living in these areas can tolerate malaria parasites without showing symptoms. Despite decades of research, we still don’t fully understand how this immune tolerance develops,” he said in an interview with the Stanford Department of Medicine. To help solve this mystery and improve vaccines and prevention strategies, his lab investigates the mechanisms behind malaria immunity.
Last year, Jagannathan’s group published a landmark study in Science Immunology, investigating the role of CD4 T cells — key players in the immune response — during malaria infections. In the study, PhD student Jason Nideffer, along with Maria Grazia Roncarolo, MD, and Jagannathan, found that T cell clones could persist in children’s bodies for hundreds of days, and re-expand upon a subsequent malaria infection. One particular subset of CD4 T cells, called type 1 regulatory T (Tr1) cells, appeared to dominate the body’s immune response, making up 90 percent of the malaria-specific CD4 T cells found in infected children.
These findings demonstrated a powerful example of immune memory, or how the immune system remembers past infections, Jagannathan told the Stanford Department of Medicine. “Although we’ve long known immune memory exists, this was one of the first times it’s been shown so clearly in humans.”
Learn more in this video.
Now, expanding upon their earlier work, Jagannathan’s team has a new research study to better understand the function and clinical relevance of Tr1 cells in children living in malaria-endemic Uganda. Their findings, currently in press at the Journal of Clinical Investigation and available as a pre-print, update existing notions of what defines a Tr1 cell, providing insights into their role in clinical immunity to malaria.
Jagannathan’s team found that Tr1 cells play a critical role in protecting children from symptomatic malaria, but they can also result in the malaria parasite persisting longer in the body through mechanisms of immune regulation.
“These findings reveal that Tr1 cells sit at the fulcrum of malaria immunity, balancing immune regulation and pathogen control,” Jagannathan said. “While this paradigm is defined here in malaria, it has relevance to other high-antigen settings such as chronic viral and parasitic infections, as well as non-infectious contexts like autoimmunity and the tumor microenvironment.”
Learn more about the Jagannathan lab’s malaria research here.