Published: 03/27/2026
By Neha Mukherjee, 2024-25 Global Health Media Fellow
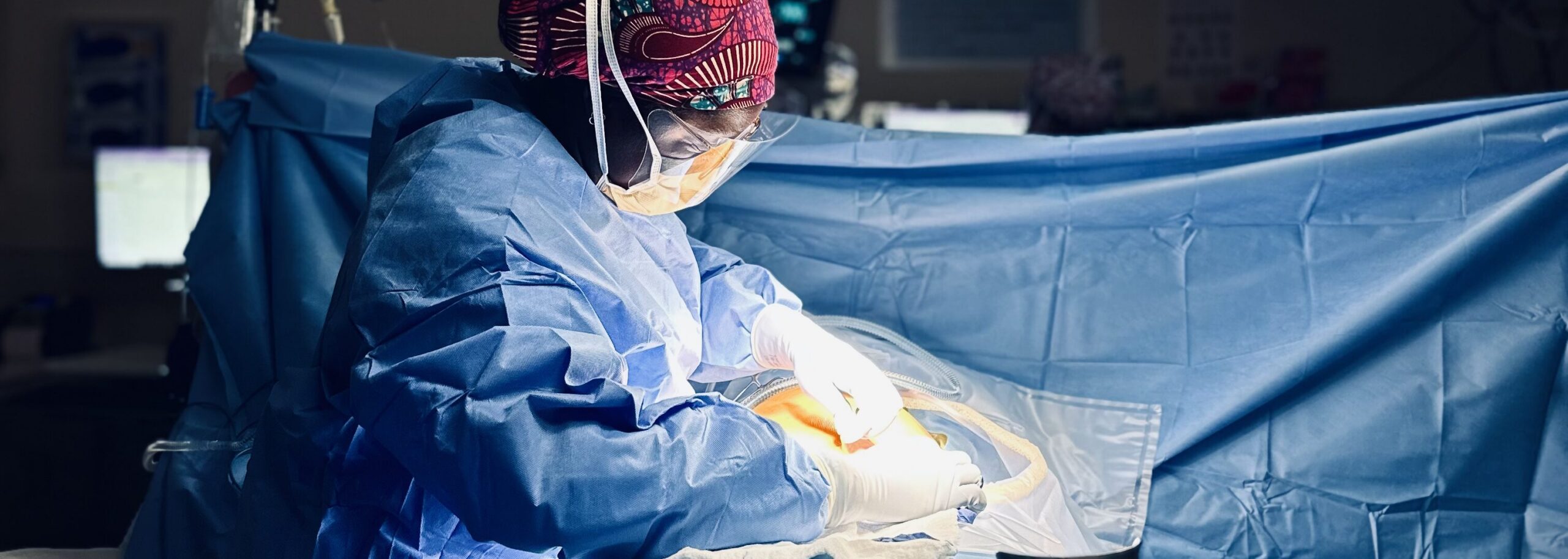
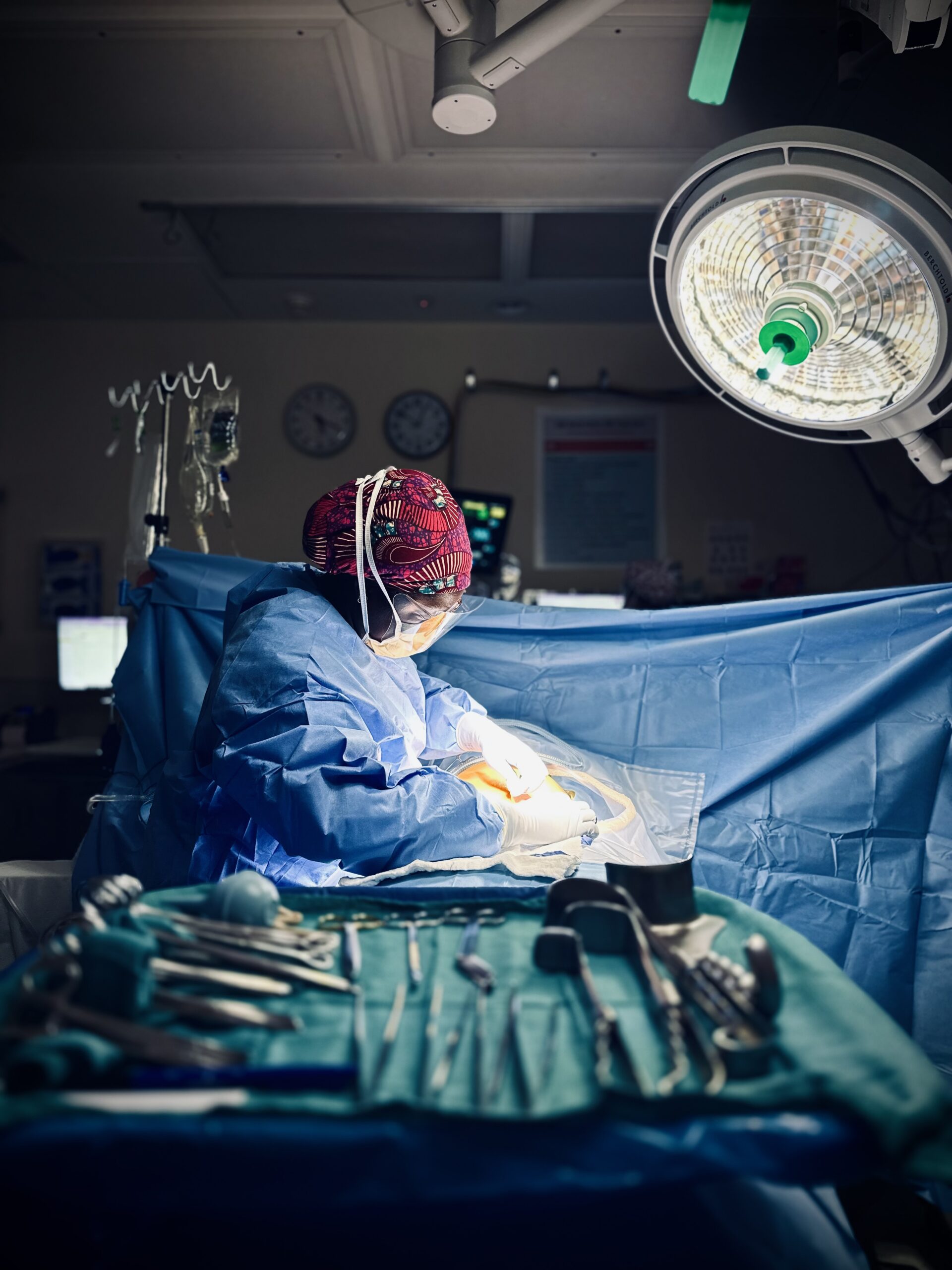
The patient was a 38-year-old female with a history of heavy and abnormal bleeding from the uterus. Dr. Metabel Markwei, her OB-GYN, explained all the treatment options. The patient chose to move forward with a hysterectomy, a complete removal of the uterus.
Markwei, a resident in obstetrics and gynecology at Stanford University, sees this type of case often. During this 2025 visit, however, she was not practicing in the Bay Area but in a more familiar place: a medical center in Ghana, close to her childhood home.
The patient was sure of her decision, telling Markwei she already had two children and was happy with that. A nearby nurse had a different opinion.
“Auntie, oh you are not done childbearing. Add one more. Add one more,” said the nurse, who then suggested that the patient might need to consult her husband first.
Markwei was shocked.
“Never in medical decision-making should a patient’s autonomy be compromised,” she says, thinking back on the encounter.
At this moment, Markwei realized that her American understanding of individual decision-making was at odds with the custom of communal input in Ghana. She recalled feeling unsure how to respond, since she was there to learn and build trust. “It was my first day on rotation, and I was plagued by the dilemma of being an observer but also a participant in care,” she said.
As she charts a long-dreamed path of practicing in both the U.S. and Ghana, while transforming her family clinic into a state-of-the-art research center, she wrestles with her dual identity as she learns how to incorporate lessons learned from both cultures into her medical practice.
“I’m in this unique position where I’m both an insider and an outsider in both worlds,” said Markwei.
Generational roots in medicine

Markwei grew up in Ghana, moving to the U.S. for college at age 17. Her passion to improve health care for African women stems from a deep family dedication to medicine. Her grandfather was one of Ghana’s first Black OB-GYNs. Her grandmother, a midwife, became president of the Ghanaian Midwifery Association. Together in 1972, the couple founded the 15-bed North Ridge Clinic, nestled in Accra, Ghana.
While her grandparents lived across the street from the clinic, Markwei lived inside of it. Her mother was a family doctor, often called to see emergency patients at night. Markwei and her family grew up in a two bedroom annex connected to the clinic by a single door, one that she opened often.
As a child, she would come home from school and help deliver meals to patients whose families lived far away. Markwei fondly remembers being the “Thursday girl,” bringing soup to patients every week and accidentally waking up sleeping newborn babies when she couldn’t resist chatting with the mothers.
It was in that same clinic where she witnessed her first childbirth, while home on break from boarding school. It was a stillbirth. Markwei remembers it vividly.
“I think that the flames of medicine were lit very early on, but I was too young to pay attention to them,” she says.
Markwei’s high school biology teacher encouraged her to apply to school abroad. She earned her bachelor’s degree in medical anthropology at Yale University, and a master’s of science from Johns Hopkins University. Then came medical school at the Cleveland Clinic, followed by Stanford University for residency. She started a Maternal-Fetal Medicine fellowship at Harvard–Massachusetts General Hospital in July 2026.
Blending medical practices across the globe

During the winter of 2025, Markwei received funding through the Stanford Center for Innovation in Global Health’s Global Scholars program to return to Ghana to complete a clinical rotation focused on women’s health.
Sometimes, resource limitations weighed heavily on the practice of medicine in Ghana, Markwei noted. She saw that sometimes blood transfusions were rationed because of lack of donor availability and handwritten referrals were used instead of electronic requests which delayed consults.
Despite these limitations, this rotation clarified her belief that health practices in countries like Ghana, can offer lessons to the wealthier countries of the Global North. For instance, Markwei observed that Ghanaian clinicians attain better diagnostic skills without reliance on more advanced medical technology: the information they garner from patient interactions and physical exams drives the diagnosis. These skills were especially useful when patients were unable to afford more expensive imaging.
Markwei was initially surprised by the use of traditional remedies, but certain cases changed her mind. One of her patients, a young woman with endometriosis causing her severe pain, reported relief after using a blend of Indian herbal products in addition to pain medication. Her story and others taught Markwei about the “interplay between anecdotal tradition and biomedicine” and sparked her desire to research the effectiveness of some of these treatments.
In the Ghanaian operating room, Markwei saw that surgical gowns and caps and some instruments could be sanitized and reused, while in the U.S. they are typically disposed of after a single use. She wondered if this sustainable practice could be used more widely across the globe.
A future of cross-country collaboration

Now, in the same clinic where she once delivered soup, Markwei wants to treat patients. She is back in the US finishing residency, but hopes to help transform North Ridge clinic into a research center by making strong partnerships globally. At a time when U.S. support for global health has been decimated, these kinds of collaborations have become increasingly threatened.
While funding is still needed, Markwei also sees this as an opportunity to re-evaluate the nature of partnerships between countries, cultivating more equitable and collaborative approaches. “This forces us to shift the way we think about global health from just aid and a top-down approach to more thinking about collaboration,” she says.
In the meantime, she is focusing on ensuring good quality care for her patients both in Ghana and the US. This includes thorough counseling, giving patients all the available information to understand a critical matter of health, or simply letting them know that they have been heard.
During her 2025 rotation in Ghana, in an ultrasound clinic, Markwei observed an encounter where a pregnant patient had asked her male physician about the sex of her baby. The doctor dismissed this request, deeming it “unimportant information.”
The patient’s demeanor changed — from excited about the new baby to saddened by the doctor’s comment and condescending attitude, Markwei recalled.
This time, Markwei stepped in.
“I’m sure it’s important for you to get ready for the baby. We will give you all of the information for you to do that,” she said.
This prompted the doctor to revisit the discussion and eventually answer the patient’s question. The patient and her husband are now excitedly preparing for a baby boy.