Published: 03/29/2021
Published on March 29, 2021
Originally published by Stanford Scope.
When COVID-19 reached U.S soil, we in the Oglala Lakota Nation carefully monitored the rising case numbers and concerning pandemic reports.
As descendants of the warriors who fought and won the Battle of the Little Bighorn, we have a history of fortitude and resilience. We trusted that we would overcome this virus.
But we were also realistic.
In the southwest corner of South Dakota, the Pine Ridge Indian Reservation is a rural community in one of the poorest counties in the country. The life expectancy is 45 years. Our health care system has little-to-no state or federal support, and this lack of public resources has long contributed to disproportionately high rates diabetes, heart disease and alcoholism.
The Indian Health Service oversees most of our medical care; but many of us questioned whether this agency of the federal government would be up to keeping the Lakota people safe during the pandemic.
Our community responded by coming together. The Oglala Lakota tribal council established a COVID-19 task force and tribal checkpoints to limit tourism on the reservation. The tribe also used KILI Radio, an Oglala-operated station, to encourage social distancing and facial coverings, and to educate community members on what to do if a loved one tested positive.
Sara J. Jumping Eagle, MD, Oglala Lakota and Mdewakantonwan Dakota, a pediatrician, is the clinical director and acting CEO of Pine Ridge’s branch of the Indian Health Service.
She recognized that if there was a surge in COVID-19 patients on the Pine Ridge reservation, the Pine Ridge Hospital medical and nursing team would need additional assistance. She reached out to several university partners. One was Stanford Medicine, where she’d earned her medical degree years ago.

A pandemic partnership
Her call was answered by leaders from Stanford’s Center for Innovation in Global Health and other Stanford Medicine faculty.
Led by Ana Crawford, MD, a clinical associate professor of anesthesiology, perioperative and pain medicine, they worked with the Indian Health Service for several months to craft a COVID-19 response, using an approach that emphasized Indigenous Sovereignty.
Rather than parachuting in and taking over, the Stanford team helped our community train and prepare for the pandemic. This ensured that our people remained empowered and at the center of the project.
As Allison Phillips, executive director of the Center for Innovation in Global Health, told me:
“We don’t think of global health as distant charity work. It is a framework for genuine partnerships to bolster health systems. The same concepts apply in our own backyard. We had an opportunity to help, and we didn’t hesitate,” said Phillips, who coordinated Stanford’s effort.

Phillips, Crawford and their Stanford colleagues began their work from afar in May. They focused on improving the hospital’s ability to treat critical care patients who would require breathing assistance, and they assessed additional needs for responding to a surge of cases.
In June, a respiratory therapist and two nurses from Stanford traveled to the reservation to create a makeshift intensive care unit and provide other assistance. They worked with the Pine Ridge Hospital team to ensure the facility had sufficient oxygen delivery supplies; and they helped train staff members in critical care management and on how to use mechanical ventilators.
Crawford told me she was impressed with the work that had been done: “Pine Ridge Hospital leadership did a great job preparing,” she said.
Rather than parachuting in and taking over, the Stanford team helped our community train and prepare for the pandemic. This ensured that our people remained empowered and at the center of the project.
For a while, it seemed that everything was going well. As of June 18, there were only 13 active COVID-19 cases in a tribal population of about 30,000.
Shelli Porter, a respiratory therapist at Stanford who traveled to the reservation, applauded the efforts.
“The uncanny low numbers of COVID-19 among the Lakota Nation spoke volumes to what the Nation was doing to prevent the spread of the virus,” said Porter, who assisted with the critical care training.
But there were things that neither the clinicians nor the Lakota Nation leaders could control.
COVID surges in South Dakota
By mid-summer, South Dakota had become a global hot spot for COVID-19.
The governor had welcomed mass gatherings and discouraged mask-wearing. In August, the Sturgis Bike Rally was held 111 miles away from Pine Ridge. More than 460,000 people flooded into the state for 10 days. Many of them refused to follow safety precautions.
Because a lot of us who live on the reservation are essential workers in nearby cities, we braced for a COVID-19 surge in our community. When it came, it lasted several weeks.
Jumping Eagle became concerned when the reservation had increasing numbers of high-acuity patients with COVID-19. She reached out to Stanford once again, requesting assistance during the surge of COVID-19 patients on the Pine Ridge reservation.
Crawford arrived at Pine Ridge in late October, with Ewen Wang, MD, a Stanford professor of emergency medicine. By then, the COVID-19 positivity rate in the community was well over 30%.
“Ordinarily, Pine Ridge can transport critically ill patients to better-equipped hospitals in Rapid City or Sioux City,” Crawford told me. “But with the surge in South Dakota, resources were limited everywhere.”
Pine Ridge needed to scale up critical-care capacity, in case other hospitals didn’t have beds available.
“We were helpful because we could train,” Wang told me. “We could help stand up an ICU.”
Holding off the pandemic
For two weeks, Crawford and Wang worked alongside Pine Ridge nurses and physicians, providing education, training and supplies in the emergency department, on the hospital ward and in the ICU.
Additional Stanford Medicine, University of Washington, Boston Massachusetts General Hospital and Society of Critical Care Medicine volunteer physicians, nurse practitioners, nurses and respiratory therapists arrived to assist with clinical care and training for varying periods of time.
The volunteers were phased down after the state’s surge had subsided and the reservation could again transfer the sickest patients to hospitals with more resources.
“The uncanny low numbers of COVID-19 among the Lakota Nation spoke volumes to what the Nation was doing to prevent the spread of the virus.”
Shelli Porter, respiratory therapist at Stanford who traveled to the reservation.
Now, the number of active COVID-19 cases on the reservation is holding steady at 30, and we are rolling out vaccinations rapidly and efficiently. Pine Ridge Hospital has collaborated closely with the Oglala Sioux Tribe COVID-19 Task Force and community programs on the COVID-19 vaccination plan and rollout efforts.
Although they are not here physically, Stanford clinicians continue to be involved. They answer questions via text and share educational resources through an online learning tool. If the need for an ICU arises again, the Stanford team is committed to reactivating the partnership.
Living on the reservation during the surge, I saw firsthand the invaluable resources provided to the hospital by Stanford and the leadership that came from within the Oglala Lakota Nation.
Our community understood our vulnerabilities, and we took action to ensure our people were well protected and cared for.
Indigenous empowerment and global health allyship held off the pandemic last year — and hopefully for good.
The warrior spirit lives on.

Anpotowin Jensen is a co-term master’s degree student in civil environmental engineering at Stanford, and is a Stanford Global Health student council member. She is passionate about elevating Indigenous and rural perspectives in global health and climate change solutions. She can be reached at sjensen3@stanford.edu.
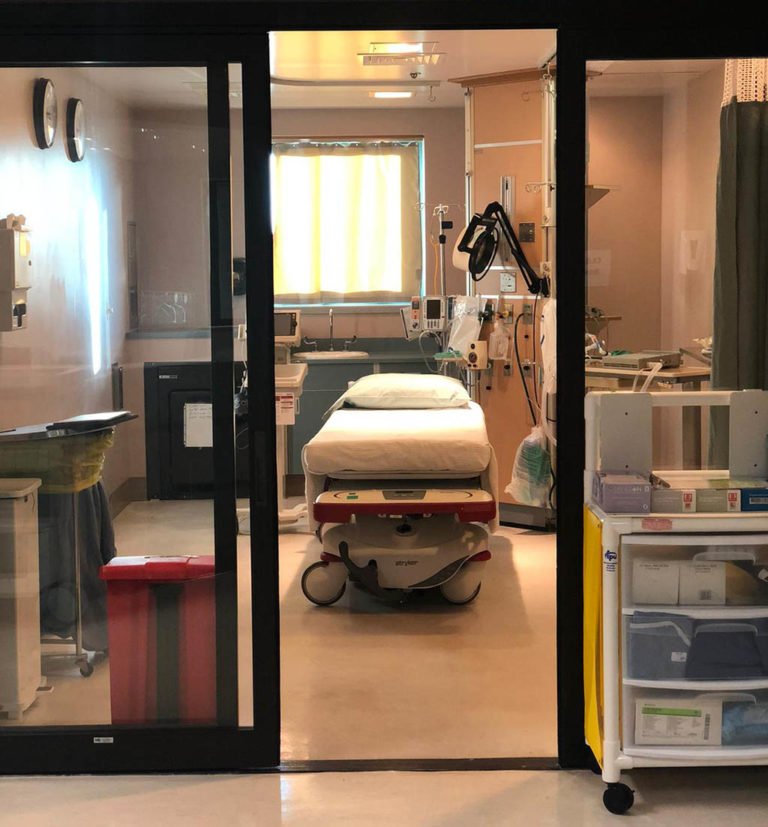
Pine Ridge Hospital entrance photos by Anpotowin Jensen. Top image and other photos courtesy of the Stanford Center for Innovation in Global Health.

