Reasons to be hopeful
Despite the global challenges of 2023, there are many reasons to feel hopeful about global and planetary health progress. We share the following stories of innovation, progress, and courage in the hope that they may help motivate and inspire renewed commitment to the much-needed global health work that lies ahead in 2024.
Caption: A barefoot solar engineer in the solar powered village of Tinginapu, in the Eastern Ghats of Orissa. By Abbie Trayler-Smith / Panos Pictures
Stories of hope and progress from 2023

Progress toward climate action at COP28

Progress toward climate action at COP28
Following a deadly summer of climate-fueled natural disasters, leaders at this year’s COP28 Summit in Dubai achieved an agreement to phase out global reliance on fossil fuels in favor of renewable energy. It was the first time that phasing out fossil fuels specifically was mentioned.
Leaders say the deal “signals the beginning of the end of the fossil fuel era by laying the ground for a swift, just and equitable transition, underpinned by deep emissions cuts and scaled-up finance.” Now comes the hard and urgent work of making this vision a reality, especially since the agreement is non-binding. Environmental, medical, and planetary health leaders can play an important role in holding countries to their promises and encouraging even swifter action.
Equally significant from a health equity and social justice perspective, leaders agreed to create a “loss and damage” fund to support vulnerable nations most impacted by climate change. Despite this landmark agreement, developed nations, including the United States, were criticized for the amount of funds they committed, which many deem insignificant to address the scope of the problem.
This year at COP28, we also saw the health impacts of climate change play an increased role in climate discussions.
Photo caption: A young girl removes snow from a solar panel at a new power plant in Balcombe, United Kingdom. Credit: 10 10 Climate Action. Via Flickr.
A newly approved vaccine aids the fight against malaria
A newly approved vaccine aids the fight against malaria
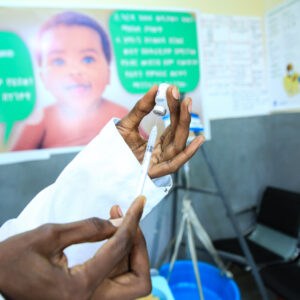
The World Health Organization has recommended a new vaccine R21/Matrix-M, for the prevention of malaria in children. This new vaccine helps address the enormous demand for childhood vaccination against this devastating mosquito-borne disease due to the first WHO-approved malaria vaccine, RTS,S, being in limited supply.
“As a malaria researcher, I used to dream of the day we would have a safe and effective vaccine against malaria. Now we have two,” said Dr Tedros Adhanom Ghebreyesus, WHO Director-General in a WHO press release. “Demand for the RTS,S vaccine far exceeds supply, so this second vaccine is a vital additional tool to protect more children faster, and to bring us closer to our vision of a malaria-free future.”
Photo caption: A doctor or nurse prepares a vaccine to deliver to a child in Ethiopia. Photo credit: Unicef Ethiopia, Flickr

A growing human and planetary health movement

A growing human and planetary health movement
Academic settings are doing more to acknowledge and address the close interconnection between the health of the planet and people, with Stanford at the forefront.
Efforts to build a new center dedicated to Human and Planetary Health, based at Stanford’s Woods Institute for the Environment and Doerr School of Sustainability, in close partnership with the Stanford Center for Innovation in Global Health and School of Medicine, moved forward this fall with the appointment of a faculty director, Steve Luby, and managing director, Allison Phillips.
The Human and Planetary Health initiative is already bringing together perspectives from environmental sciences, public health, systems thinking, policy, law, and other disciplines to achieve breakthroughs and find solutions that protect human health and address climate change.
Also this year, CIGH launched Medicine for a Changing Planet, a new online portal offering new educational resources to support health care providers in responding to emerging health threats caused by climate change and other environmental challenges. This tool was developed in partnership with the University of Washington’s Center for One Health Research and is free and accessible to all.
Read more about Medicine for a Changing Planet.
Read more about the Human and Planetary Health Initiative at Stanford.

A low-tech way to save millions of newborn lives

A low-tech way to save millions of newborn lives
Nearly 1 million preterm infants die each year from complications. As a pediatrician, Core Leader Dr. Gary Darmstadt sees those lost lives as unacceptable and, in many cases, preventable.
As co-chair of a WHO guideline development group, Darmstadt has spent years helping to develop the evidence base to inform new recommendations for measures that can, collectively, prevent nearly three-fourths of newborn deaths.
Key among them is centering mothers and families in the care of their preterm infants – including the use of Kangaroo Mother Care. Darmstadt also co-chairs a WHO Strategic Technical Group of Experts on Kangaroo Mother Care. This group has also published a research agenda, a Global Position Paper, and an Implementation Strategy for advancing this life-saving care.
Photo caption: Kangaroo Mother Care inside Assosa General Hospital. UNICEF Ethiopia/2017/Meklit Mersha

A sustainable solution to period poverty

A sustainable solution to period poverty
For people who menstruate, access to affordable and hygienic period products is a necessity. A lack of pads, tampons, menstrual cups, or safe and hygienic facilities to use and dispose of them can affect attendance at work and school or participation in other aspects of daily life. Yet studies estimate that 500 million people – women, girls, and transgender and nonbinary individuals – don’t have access to the facilities and products they need to manage their period.
Researchers at Stanford, including Global Health Core Leader Dr. Manu Prakash, have designed an open-source process for turning sisal fibers into absorbent material for menstrual pads, creating an opportunity for the local, sustainable manufacture of hygiene products that many communities need.
Read the full story by LAURA CASTAÑÓN.
Photo credit: Andrew Brodhead, Stanford

Accelerating cervical cancer prevention in Nigeria

Accelerating cervical cancer prevention in Nigeria
Global Health Core Leader in Oncology, Dr. Ami Bhatt, shared a story of hope from Nigeria.
Nigeria, Africa’s most populous country, this fall introduced the HPV vaccine into its routine immunization system, aiming to reach 7.7 million girls age 9-14 in the largest single round of HPV vaccinations across Africa.
The vaccine prevents infections with certain strains of the human papillomavirus, the most common cause of cervical cancer. Program leaders say the vaccine could ultimately help save millions of lives in a country where cervical cancer is the third most common cancer and the second most frequent cause of cancer deaths among women aged 15 – 44.
“This is a major step forward in preventing the 8,000 deaths per year that occur in the country due to cervical cancer,” said Dr. Bhatt. “I am so thankful to colleagues at Stanford, our nonprofit Global Oncology, our Cervical Cancer Free Nigeria ambassadors, and beyond for helping to make this happen!”
Photo credit: A mobile clinical outreach team visits Laniar health center to offer many sexual reproductive health services including cervical cancer screening and treatment. From Imagesofempowerment.org.
Paving the way for safer surgery
Paving the way for safer surgery
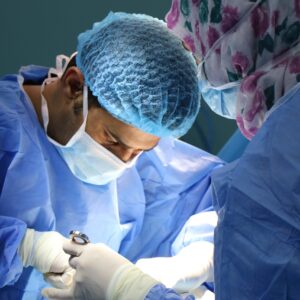
The right to access safe, equitable surgical care is unfortunately out of reach for millions of people around the world, writes our colleague at Stanford Surgery’s Office of Global Engagement.
Now, Core Leader Dr. Tom Weiser and Global Health Equity Scholar Maia Nofal are teaming up with Lifebox, a charity focused on improving safe surgery and anesthesia globally, to tackle these inequities.
The team is using a global health seed grant award to investigate a particular challenge of safe surgery: preventing infection while avoiding unnecessary antibiotic use, which can lead to dangerous antimicrobial resistance. They’re using the seed grant to test the efficacy of an “Antibiotic Timeout” to reduce unnecessary perioperative antibiotic use in Ethiopia, Malawi, and Rwanda.
Learn more about Dr. Nofal’s work and this promising frugal innovation.
Photo credit: Jafar Ahmed, Unsplash.com

Transporting critically ill children from conflict to care
Transporting critically ill children from conflict to care
Global Health Core Leader Dr. Paul H. Wise is committed to ensuring that children with cancer and other critical illnesses receive the life-saving care they need and deserve, regardless of their surrounding circumstances.
Since 2022, he has been helping to coordinate the evacuation of pediatric cancer patients in Ukraine, along with their families, so that the children can receive the care they require in other countries. To date, they’ve helped about 1,500 children.
Photo: An ambulance in Gaza in 2009. By Gigi Ibrahim via Flickr

Expanding global access to critical care

Expanding global access to critical care
Robust emergency, critical care, and operative care are critical to a nation’s ability to meet its citizens’ health needs, especially during emergencies such as pandemics and natural disasters. And yet, COVID-19 revealed significant gaps in how these services are provided, which resulted in many lost lives.
While critical illness is common, 90 % of critically ill patients receive care outside of intensive care units. This challenge is not unique to emergencies, said Dr. Ana Crawford, Director of Global Engagement Strategy in Stanford’s Anesthesiology & Critical Care Medicine Department. She noted that patients become critically ill every day, yet often do not receive the timely care they require due to a lack of, or delayed, recognition of their illness.
“Morbidity and mortality are unacceptably high for critically ill patients — a situation that becomes even more dire when health systems are strained,” she said.
Now, an international resolution seeks to address that. At the 2023 World Health Assembly, member states for the first time vowed to strengthen healthcare systems’ capacity to serve critically ill patients by expanding emergency, critical, and operative care.
The resolution calls on Member States to create national policies for sustainable funding, effective governance and universal access to needs-based services for all; to promote integrated delivery of these services within relevant national health system assessments and strategies; and to promote more coherent, inclusive and accessible approaches to safeguard emergency services in disasters, fragile settings and conflict-affected areas. Read more here.
The Global Anesthesia and Critical Care Learning Resource Center created under Dr. Crawford’s leadership now offers a free online continuing medical education course, which educates professionals about Essential Emergency and Critical Care. Learn more.
Photo credit: Robert Linder, Unsplash.com

