Published: 01/30/2024
Stanford Surgeon Sherry Wren’s International Humanitarian Surgical Skills Course, now in its tenth year at Stanford, has equipped hundreds of surgeons and healthcare providers with the unique skills and knowledge they need to save lives in conflict zones and low-resource settings.
By Maria Isabel Barros Guinle, Stanford Medical Student, with contributions from Jamie Hansen, Global Health Communications Manager
In 2006, Stanford surgeon Sherry Wren, MD, was on her first of many trips with Doctors Without Borders in Cote D’Ivoire, amid a civil conflict. A man came to her clinic with an infected effusion of his chest, unable to breathe properly. He needed a chest tube, but when she placed it, she realized that the facility did not have the chest drainage system required to pull the pus from his lungs. These machines use wet and dry suction to create a positive pressure which allows for fluid to drain out of the lungs. They cost around $60 — a price too steep for hospitals in conflict zones.
“I thought, ‘what in the world am I going to do?’” she recalled. “And then I realized, this is all I have. I’ve got to make it work.”
“I thought, ‘what in the world am I going to do?’ And then I realized, this is all I have. I’ve got to make it work.”
Sherry Wren, MD, Leader of the International Humanitarian Surgical Skills Course
She had a urinary catheter bag, but it did not allow for air draining. So she improvised, flipping the bag upside down to allow the air to vent off. Instead of using a sterile water system through which air bubbles can travel up to prevent air locking and increased pressure in the patient’s chest, she used the pus coming out of the patient to her advantage to create a wet suction system. The system allowed air to vent off and bubble through, preventing air locking — an invention of necessity she dubbed the pus-o-vac.
Not long after returning from trip, Wren, a professor of general surgery at Stanford Medicine and core leader at the Stanford Center for Innovation in Global Health, began to develop a one-of-a-kind course to teach others the skills she wished she’d known.

Over the weekend of Jan. 20 and 21, 45 physicians and advanced practice providers gathered for the International Humanitarian Surgical Skills Course, now in its 10th year at Stanford, where it is hosted in partnership with the Stanford Center for Continuing Medical Education. Inside Stanford’s anatomy lab in the Li Ka Shing Center, physicians could be seen practicing skills such as how to manually drill holes into cadaver skulls as they prepared to manage traumatic brain injuries in low resource settings across the globe.
“This class teaches the skills you can’t learn by doing them here in the U.S,” said Wren. “It’s a combination of what I wish I’d known when I began working overseas and what is possible to teach.”
“This class teaches the skills you can’t learn by doing them here in the U.S. It’s a combination of what I wish I’d known when I began working overseas and what is possible to teach.”
Sherry Wren, MD
In the last 14 years since its creation in 2010, the course, which Wren also teaches at for the American College of Surgeons, has served an estimated 800 participants from the United States and overseas from Canada to Madagascar. Since its inception, it has become a go-to resource for surgeons and other medical professionals seeking to gain skills to help them serve patients in settings where resources are scarce.
Participants have included pediatricians, trauma surgeons, neurosurgeons, internists, and physician assistants, among others. Some attendees practice not overseas, but in rural areas in the United States where there are few specialists and the skills learned in the course can benefit their local population.
Wren recalls that one former participant from a very rural region of Texas used basic flap techniques he learned during the training to do skin cancer excisions locally, rather than refer his patients far away for care.
This winter’s one-and-a-half-day course began with introductory lectures and was followed by skills sessions in which attendees practiced implementing some of the most common surgical techniques in low-resource settings, from hand injuries and burns, to blocked prostates, to obstetric emergencies. During her opening remarks, Wren emphasized the physical and emotional toll these humanitarian trips can have on physicians. She expressed that developing this course helped her process the emotions she has felt while providing care overseas.
The training, Wren emphasized, isn’t just about teaching physical skills. Wren and her co-instructors strive to impart the mindset of safety and responsibility.
“You have to realize you’re not at home; you don’t have the resources that you’re used to, and you’d better know what supplies you have to work with,” she said. “You’d better know when not to do something, because you can’t transfer somebody if things go wrong.” Preparation also includes understanding the cultural, ethical, and legal context of the country and registering with the state department and having an evacuation plan – particularly in unstable countries.
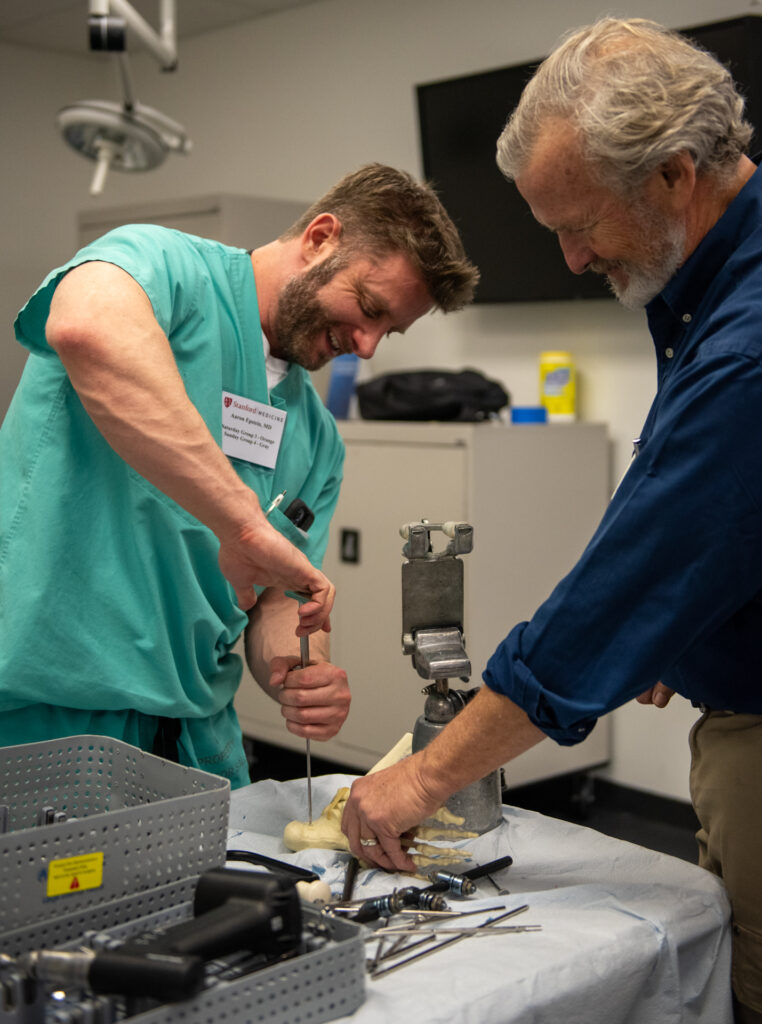
The close teacher-to-student ratio sets this course apart from others. Instructors include volunteer Stanford faculty from numerous medical departments and other medical experts, some of whom fly in for the occasion, to share their expertise in the techniques covered. This year, speakers included Dr. Clifford Sheckter; one of very few double-board certified physicians in both Surgical Critical Care and Plastic and Reconstructive Surgery. Sheckter led a session about complex wound care in low resourced environments in which burns can be common but standard treatments are unavailable. His talk was followed by lectures by medical experts in anesthesia, infectious diseases and tropical medicine, and orthopedic surgery.
Lectures on Saturday were followed by afternoon skills sessions in which participants practiced critical surgical skills they may need in these environments. Stations covered how to perform external fixations for orthopedic emergencies, skin grafts and flaps for wound care, management of hand injuries, and burr holes for traumatic brain injuries. These sessions covered a wide range of skills because some of the attendees are not surgeons, and those who are surgeons may need to learn skills outside of their subspecialty.
Sunday sessions included more hands-on practice focused on obstetric and gynecological (OBGYN) emergencies. Five skills stations allowed patients to practice performing emergency c-sections, uterine evacuation, controlling post-partum hemorrhage, and using intrauterine tamponade devices. Wren explained that many women in low-resource settings suffer miscarriages, birth complications, and can die during childbirth, so OBGYN skills are crucial. Wren recalls when she had to perform a C-section on the wife of a village leader during one of her trips.
“I know I can’t do complicated vaginal deliveries, but I am a surgeon, and a c-section is a surgery that can get the baby safely out. That’s something I can do,” recalls Wren.
Even though general surgeons are not normally tasked with performing cesarean sections in the United States, in conflict and low resource zones, they may be the only doctors available. Having the skillset to deliver a baby can save two lives at once.
Course attendee Aaron Epstein, a general surgery resident at the University of Buffalo, took the course to supplement the knowledge he has acquired by providing medical aid abroad in Iraq, Ukraine, South America, Africa and other locations throughout his residency.
“A lot of times these surgeons are expected to handle everything that gets thrown at them. Learning the skills in this course … you can actually handle a lot of what comes through in these emergency settings.”
Aaron Epstein, General Surgery Resident at University of Buffalo
“A lot of times these surgeons are expected to handle everything that gets thrown at them,” he stated. “Learning the skills in this course … you can actually handle a lot of what comes through in these emergency settings.”
Epstein, who will begin his trauma fellowship later this year, hopes to continue to provide care in low-resource settings that lack medical care.
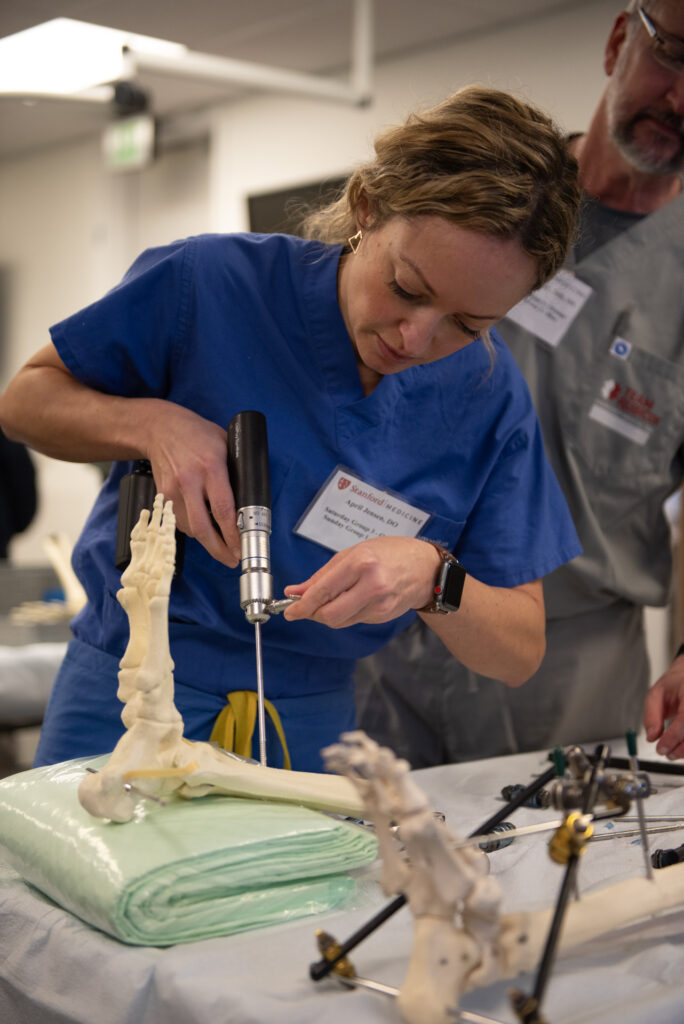
April Jensen, a practicing general surgeon in Albany, Oregon, takes trips each year to provide surgery in other locations and sought out the training after she started a surgical nonprofit.
“I was looking for something where I would get some hands-on skills and also meet other people with similar interests,” she said.
While rotating through different stations, participants discussed their backgrounds and connected over their shared commitment to provide surgical care to people who need it around the world. Physicians of different specialties exchanged knowledge about their areas of expertise and helped each other learn new skills.
Wren said she often receives emails from course alumni letting her know they’ve put a skill they learned in the course to use. “I’ll hear from people who are working overseas, and because of what they learned in the class, were able to take care of a patient safely,” she said. “That’s amazing to hear.”

