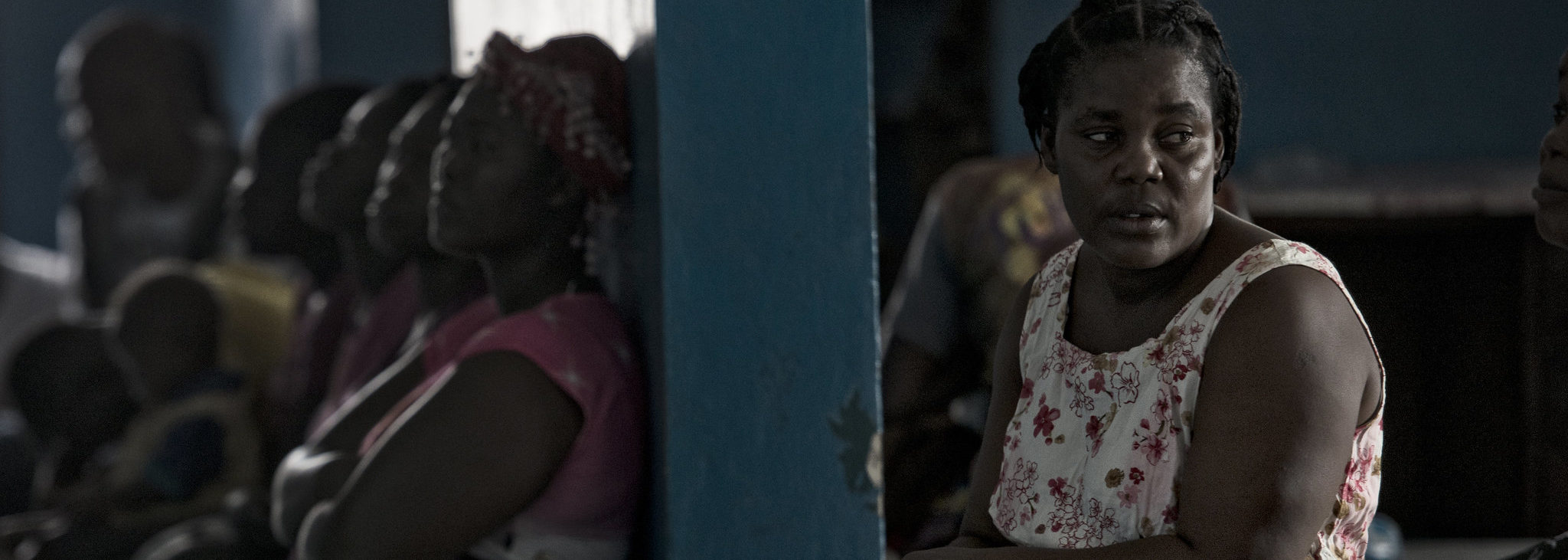Published: 07/08/2021
Can improving natural ventilation in hospitals in Liberia make its health care systems more resilient to emerging infectious diseases? This new project seeks to find out. Healthcare facilities in low-resource settings, like Liberia, are often under-prepared to prevent disease spread among patients or healthcare workers, particularly when faced with airborne diseases like COVID-19 and tuberculosis. Liberia is a key hotspot for emerging infectious disease and tuberculosis is a significant concern there. Improving ventilation is critical to reducing hospital-acquired airborne infections.
Despite this, much of the current research has neglected to focus on natural ventilation in favor of mechanical ventilation, which is not always available in low-resource settings due to cost, electricity, and required engineering expertise. Researchers will use carbon dioxide levels as a proxy for airborne infectious disease transmission risk to identify potential hot spots in hospitals and study the effectiveness of natural ventilation methods like window exhaust fans and skylights in Liberia. Researchers hope to identify cost-effective structural changes that can improve ventilation and design a CO2 monitoring system that can visually display ventilation status.
“By identifying low-cost strategies for optimizing ventilation in naturally-ventilated healthcare facilities, we will strengthen the resiliency of healthcare facilities and protect healthcare workers and patients against endemic and pandemic airborne infectious disease spread.”
Co-PI Jorge Salinas
“By identifying low-cost strategies for optimizing ventilation in naturally-ventilated healthcare facilities, we will strengthen the resiliency of healthcare facilities and protect healthcare workers and patients against endemic and pandemic airborne infectious disease spread,” said Co-PI Jorge Salinas.
Principal investigators: Jorge Salinas, Thomas Michael Baer
Photo credit: Neal Brandvold for USAID, Flickr