Published: 08/17/2020
Dear Global Health Colleagues,
With more than 200 COVID-19 vaccines barreling towards deployment and Russia approving an untested vaccine last week, the global attention has shifted towards vaccine safety, allocation and efficacy. China and the US continue to be locked in a competition that has caused worry of premature release of vaccines before safety has been established. I therefore thought a newsletter devoted to vaccines is timely.
A fast track National Academy of Medicine (NAM) committee on equitable vaccine allocation chaired by Helene Gayle and Bill Foege (both of whom have spoken at Stanford Global Health events) has been assembled by the global health board I sit on to discuss safety and allocation issues. A recording of their first meeting, open to the public, is available here.
Vaccine development is unfortunately only the beginning of our concerns, as is well-depicted in this eye-opening article from the Center for Strategic and International Studies. There are greater forces at play outside of the laboratory that demand our attention, much of which depend on the imminent action of the United States and a few other key players.
An alarming outcome awaits a failure to unite in a coordinated vaccine development and deployment strategy. An “us first” vaccination mentality would prove disastrous: extreme nationalism drives vaccines towards countries of wealth and clout while failed international cooperation stymies crucial supply chains. “It means that every nation, instead of cooperating as we hope they will, instead decides to compete and prioritize their own people first,” says Stanford Global Health Faculty Fellow David Relman, M.D., in this article from ABC.
I choose to believe in a brighter future, one that the COVAX initiative is well positioned to forge, both for the United States and the world. Co-led by Gavi, CEPI, and the WHO as a cooperative of countries working on vaccine trials, COVAX would pool resources and coordinate financial incentives to bring as many vaccines into use as quickly and equitably as possible across the globe. COVAX is still underfunded.
We should advocate for the US to contribute to this fund, and we must continue to deploy the only effective and available interventions we have to prevent this deadly virus: masks, social distancing, good hygiene, and testing, tracking and isolating all cases. Lastly a vaccine is only effective if people take it and have confidence in its efficacy and lack of adverse effects. Sadly, a US poll showed only 43% of people reporting they would take the vaccine. In the fall we will be conducting a global conversation with Heidi Larson, a world renowned anthropologist from the London school of tropical medicine and hygiene who studies vaccine confidence—more updates to come.
We hope you review the articles and resources below which guide us towards the only successful conclusion to the COVID-19 pandemic, an equitable one.
In solidarity,
Michele Barry
Drs. Ben and A. Jess Shenson Professor of Medicine and Tropical Diseases
Director of the Center for Innovation in Global Health
Senior Associate Dean for Global Health, Stanford University
Resources
COVID-19 Vaccines
- Immunogenicity and safety of a recombinant adenovirus type-5-vectored COVID-19 vaccine in healthy adults aged 18 years or older: a randomized, double-blind, placebo-controlled, phase 2 trial (8/15/20): Phase 2 trials of the Chinese vaccine, described.
- Researchers Strive to Recruit Hard-Hit Minorities Into COVID-19 Vaccine Trials (8/13/20): With communities of color far over-represented in the COVID-19 infection and death numbers, diversity is essential in the vaccine trials, but willingness to participate is low due to a deeply troubled history of medical exploitation.
- Evaluating use cases for human challenge trials in accelerating SARS-CoV-2 vaccine development (8/6/20): JID article evaluating the efficacy and ethical issues of human challenge studies which will give an efficacy answer way faster than randomized trials. This has been done with other vaccines but there has always been a rescue therapy.
- The rush to create a covid-19 vaccine may do more harm than good (8/5/20): An important reminder of the potential pitfalls of a rushed vaccination process in the BMJ Opinion.
- Ensuring Uptake of Vaccines against SARS-CoV-2 (7/14/20): An NEJM article from Stanford Global Health Faculty Fellow Michele Mello on ensuring vaccination uptake through 6 proposed trigger criteria that must be met.
Regional News
- Guidelines for Healthy In-Person Voting (8/12/20): The Brennan Center for Justice’s guidelines for safe voting, a critical consideration for the upcoming election, which I had the honor to advise on.
- New Zealand on alert after 4 cases of COVID-19 emerge from unknown source (8/11/20): New Zealand’s director-general of health is quoted in this article saying, “This case is a wake-up call against any complacency that may have set in,” reminding us to keep our guard up in all conditions.
- The pandemic appears to have spared Africa so far. Scientists are struggling to explain why (8/11/20): Confounding test results coming out of Africa are provoking interesting discussion of causes and possible courses of action, including waiting for herd immunity.
- Fighting for breath: How the medical oxygen industry is failing African hospitals (8/10/20): Oxygen in sub-Saharan Africa is five times more expensive than in the US or Europe — a price that is costing lives.
Underserved Populations and Health Disparities
- Climate change and COVID-19: Reinforcing Indigenous food systems (8/7/20): This comment in the Lancet uses the microcosm of the pandemic to dissect the larger trends of dismantling indigenous food systems, the vulnerabilities this process creates, and the potential resilience and health outcomes of their recovery.
- Potential effects of disruption to HIV programmes in sub-Saharan Africa caused by COVID-19 (8/6/20): It is important not to overlook the existing pandemics during COVID-19 — this model shows how even a brief interruption in HIVservices may put millions of people at severe risk.
Notes from the Field: : India & Bangladesh

Shahed Alam, Co-Founder, Noora Health, Stanford School of Medicine ’11
Edith Elliott Queeney, Co-Founder, Noora Health, Freeman Spogli Institute ’10
Noora Health was founded with the mission of bringing family caregivers to the center of healthcare delivery in India and Bangladesh, by two Stanford students and funding from a Stanford Global Health seed grant.
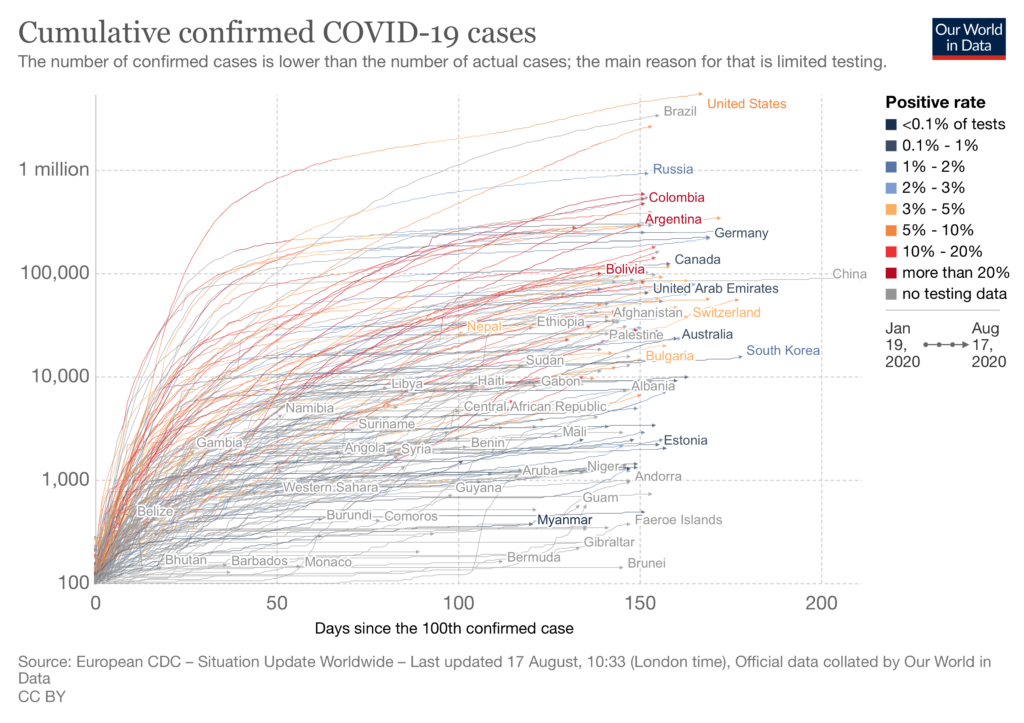
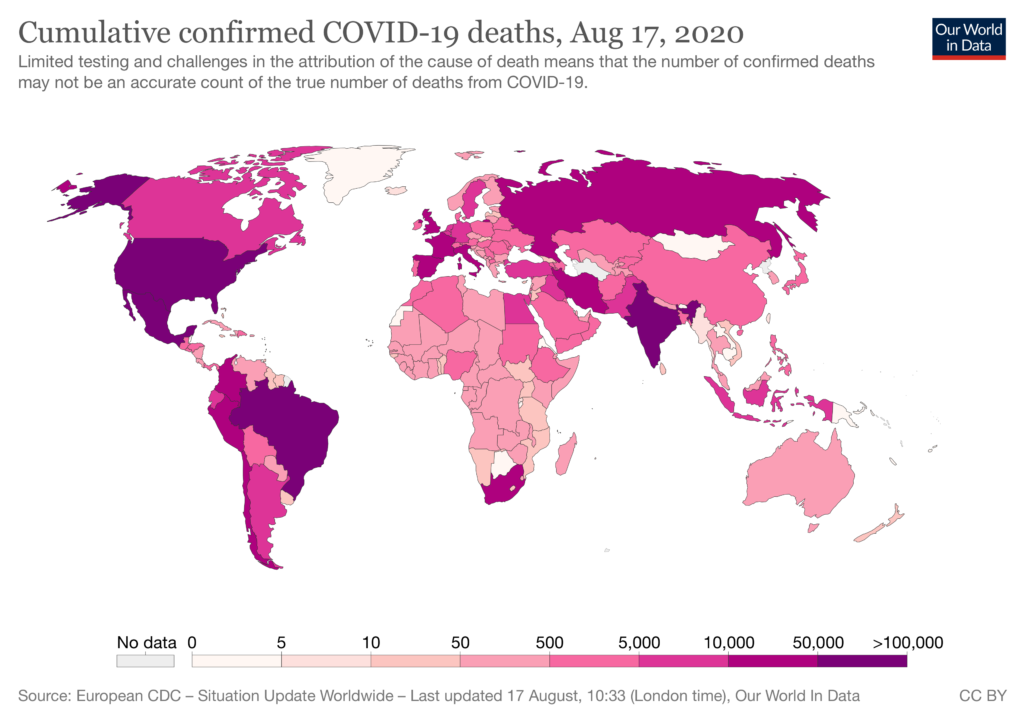
When COVID-19 hit, Noora Health adapted its model to support communities and health systems in a region where the virus had the conditions to rapidly spread with devastating consequences. Unfortunately, India currently records the highest number of daily COVID-19 cases worldwide.

We began our response in March. With a pool of more than 6,000 individuals across the region, we conducted research that yielded unsettling results: people felt they knew enough about COVID-19 and had received plentiful information, yet the actual practice of preventive behaviors was a mixed bag. Moreover, the public’s risk perception of actually being able to contract the disease was very low. From our qualitative studies, we understood that people were saturated with information from various sources.
Our job was to break through the noise with the right messages. We began to train trusted community members who were not previously involved in health, like frontline workers of microfinance institutions. These individuals were able to contextualize and drive accurate health messaging in the communities they belonged to.

Eventually, one of the unintended consequences of initial COVID-19 information campaigns was excessive fear of the disease. This fear fueled stigma that was caused by a multitude of additional factors – including local social ostracisation of positive patients. This leads to populations under-reporting symptoms and not cooperating with public health measures. We must now evolve our messaging to understand the nuance between instilling seriousness and appropriately normalizing the disease.
COVID-19 has challenged the fragile health system in this region. New care models have long been needed, and our original thesis – that health happens at home – still rings true. We have partnered closely with several government institutions to remotely train family caregivers of COVID-19 positive patients and other high risk groups to keep them safe at home. We’ve seen the evidence of impact when primary care models recognize the need to empower families to care for their loved ones, and we’re optimistic that this focus can lay the groundwork for strengthening health systems.

Stanford Global Health Updates & Opportunities
Global Health Equity Scholars (GHES) Fellowship
The Global Health Equity Scholars (GHES) Fellowship is currently receiving applications for a one-year mentored research training program for post-doctoral fellows, upper-level PhD students and professional school (MD, DVM, DrPH, PharmD) students in low- and middle-income countries. The GHES Fellowship is part of the Global Health Program for Fellows and Scholars sponsored by the Fogarty International Center (FIC) and several collaborating institutes and centers at the National Institutes of Health (NIH). The deadline for applications is November 2, 2020. For more information contact Stanford GHES Program Manager Olivia Paige at olivia.paige@stanford.edu or visit this page.
Fogarty-Fulbright Fellows in Public Health Program
The Fulbright US Student Program is currently receiving applications for the Fulbright-Fogarty Fellows in Public Health. The purpose of the program is to promote the expansion of research in public health and clinical research in resource-limited settings. The deadline for applications is October 13, 2020. Please note that the internal university deadlines for Fulbright are earlier than the October date (Stanford deadline: September 13, 2020). For more information contact Olivia Paige at olivia.paige@stanford.edu or visit this page.
Upcoming Events and Lectures
Stanford Medicine Grand Rounds: The COVID 19 Pandemic through a Gendered Lens
Wednesday, August 19, 2020 | 8:00 – 9:00 am PT
Stanford Department of Medicine
Event information and registration.
Director of Stanford’s Center for Innovation in Global Health, Dr. Michele Barry presents at this week’s grand rounds, highlighting the gendered components of the ongoing pandemic.
Gender & Power: Exploring Women’s Voices and Representation in MediaThursday, August 20, 2020 | 8:30 – 9:30 am PT
WomenLift Health
Event information and registration.
Women have long been underrepresented in the mainstream media – as journalists, editors and opinion writers, as spokespeople and quoted experts, and as subjects of stories. During the COVID-19 pandemic these disparities have only been exacerbated. Male voices have dominated the public narrative about the pandemic, building on a longstanding culture of media turning to men as the leading figures of scientific authority. Women, for example, make up only a handful of those quoted in coverage about COVID-19. Thinking about how diversity in media enhances our ability to understand the impacts of health emergencies like COVID-19 is critical. Hear from three leading women in health media on the various ways gender disparities play out in the field, how women are changing the landscape, and the critical steps media institutions can take to ensure equitable representation throughout all aspects of their organizations.
How Pandemic Response Can Inform the Path Forward
Wednesday, August 26, 2020 | 10:00 – 11:30 a.m. PT
Stanford Woods Institute for the Environment
Event information and registration.
COVID-19 is a monumental public health crisis, with a grim toll in lives lost and economies disrupted. But the pandemic has also produced ripple effects that are challenging social norms and allowing governments and businesses to reimagine how they operate. Climate change impacts are unfolding over a longer time horizon, but are expected to be similarly disruptive and massive in scale. What lessons learned from the pandemic will contribute to a better future? What opportunities have revealed themselves and what will it take for change to last? Join Stanford faculty as they engage each other in conversation around these thought-provoking, interdisciplinary questions informed by approaches in economics, earth system and environmental science, behavior and decision making science, and political science.
NorCal Symposium on Climate and Pandemic Resilience in Health Care
Friday, September 25, 2020
Stanford Medicine and UCSF
Event information and registration.
The symposium, co-sponsored by the Stanford Center for Innovation in Global Health, will educate and empower health care professionals to enact sustainable healthcare practices at their institutions. The COVID-19 pandemic has laid bare the vulnerabilities of health care systems in the US to adapt and mobilize resources needed to provide timely, appropriate, and equitable care. Climate change adds stressors such as wildfires, super storms, and heat waves that further test our capacity. It is critical that we build resilient health care systems, able to respond effectively in times of crisis. Through interdisciplinary sessions with health care workers, sustainability officers, and advocates for sustainable solutions, we will build a community of invested individuals and organizations to create resilient and equitable health care systems.
Women Leaders in Global Health Conference 2020
October 13-15, 2020
WomenLift Health
Event information and registration.
This year’s conference will take place in a virtual format, with three hours of dynamic sessions and speakers each day. There will be two distinct days on women’s leadership in South Asia and Africa, culminating in a day of global dialogue. While the geography-specific days are geared toward South Asia and Africa through both timing and focus, these sessions are open to everyone. The theme of this year’s conference is Connect | Commit | Act. We believe that by coming together, we can shape a collective vision for global health, where diverse women have a seat at the decision-making table.
New Funding Opportunities Specific to COVID-19
SPARK Translational Research Program Pilot Grants – Request for Proposals
Available to Stanford researchers only. The Stanford SPARK program supports the discovery and development of novel therapeutics and diagnostics that address unmet medical needs. SPARK offers funding, education regarding the multi-disciplinary product development process, and project-specific mentorship to enable faculty and trainees to advance promising research discoveries to the clinic and/or commercial sector. Much of the mentorship and education is provided by volunteer advisors from the local biotechnology ecosystem. Education and mentorship are available across the entire spectrum of drug and diagnostic development including the following areas: intellectual property and patent law; assay development; optimization of therapeutic chemical structures; preclinical pharmacology and proof of concept studies; preclinical safety and pharmacokinetics; regulatory science and regulatory agency expectations; clinical study design and conduct; and commercialization/start-up company funding and incorporation. Approximately 60% of projects that complete SPARK advance to commercial partnerships and/or clinical trials. More information Here.
Online List of COVID-19 Funding Opportunities
Stanford’s Research Management Group has created a website that provides a complete listing of funding opportunities for COVID-19 research available to all researchers (not just at Stanford). More information here.
CIGH Faculty Fellow’s Global Research on COVID-19
digitalMEdic — COVID-19 Trainings for Healthcare workers: Stanford’s Global Emergency Medicine Department and Digital Medic Create New Education Tools for COVID Patient Care