Published: 02/21/2020
By Jody Berger
When Sherry Wren, MD, treats patients at the Stanford Hospital, she has a top-notch team around her, the latest technology at her fingertips and the confidence that comes from years of experience providing surgical treatment for gastrointestinal cancer.
However, when Wren travels overseas to provide humanitarian surgical care in conflict zones things rapidly change. On these trips, she may not know the team (if there is one); she may be missing basic surgical instruments; and she will be called on to care for any and every type of patient.
“The most common operation I’ve done in that setting is a Caesarean section because pregnant women frequently have obstructed labor when the baby can’t exit the birth canal,” she said. “I once did 70 Caesarean sections in a four-week time period.”
Wren started volunteering with Doctors Without Borders in 2006. After a few trips with the international nonprofit, she thought about what she wished she’d known before going and what skills she’d like to have on future trips. The reflection prompted her to design a course for surgeons like her: men and women who want to help the patients in foreign lands who don’t have consistent access to medical care.
“I thought it was important to take high-resource surgeons and teach them how to go low-resource,” Wren said in the opening talk of this year’s course, the tenth annual International Humanitarian Surgical Skills Course.
Wren is a professor of surgery and a member of the leadership team for Stanford’s Center for Innovation in Global Health. She initially designed the two-day course for general surgeons but routinely finds herself teaching medical practitioners with a variety of specialties and subspecialties. This year’s class included family medicine doctors, pediatricians, gynecologists, internists, anesthesiologists, as well as nurse practitioners and physician’s assistants.
“I’m not here to tell you the right answer,” Wren told them. “A lot of times, there is no right answer but you’ll have to make the best of it.” She also stressed that decisions must be made taking into account the specific resources on hand such as medications, supplies, blood, and staff.

Wren shared practical tips for traveling overseas, including which socks to wear (she likes Sockwell) and what to drink. “I don’t drink water if I don’t see them boil it but remember,” she said, “beer and soda are both sterilized water.” She also listed medications to carry, instruments to bring and added, “Duct tape is a miracle.”
In a series of case studies, Wren illustrated the need for MacGyver-level improvisational skills and a willingness to make tough decisions.
When the patient is a 5-year-old boy with a soft tissue sarcoma—something that is highly treatable and often curable—what should a doctor do if she has no access to chemotherapy or radiation?
What if the patient is a pregnant 22-year-old woman who desperately needs a C-section but lives in a culture where only her husband can give consent and he won’t?
Or what should a physician do if the patient is a 7-year-old boy who’s been raped by a family member but there is no Child Protective Services to call?
“You will feel psychic pain,” Wren told course participants.
And for some of the participants, the course may show that they don’t want to practice medicine in these situations. The lectures and photos may be enough to dissuade them and Wren’s okay with that outcome. “It’s not for everyone,” she said. “And I want them to know what they’re getting into before they go.”

For other participants, the course is just the beginning. Gail Rosseau, MD, is a Clinical Professor of Neurosurgery at George Washington University in D.C. Three years ago, Rosseau emailed Wren to ask if neurosurgeons were welcome. And once she took the course, Rosseau decided to recreate it for her own discipline.
“Two-thirds of the people on the planet don’t have access to emergency and essential surgery,” Rosseau said. “In my own discipline of neurosurgery that means we need 23,000 more neurosurgeons today to be able to handle the operations that aren’t being done because there aren’t people out there.”
Rosseau didn’t want to retrain everyone to do everything, but she knew there were board-certified neurosurgeons with transferrable skills who could benefit from a refresher course to reclaim the skills they once had but aren’t part of their daily practice. She offered the course for the first time at the American Association of Neurological Surgeons annual conference and hoped to have 32 participants. She ended up with 57 neurosurgeons in attendance.
Rosseau also committed to sharing her skills with students in Wren’s course. The first day, she taught the skills station on burr hole craniectomy with Stanford neurosurgeon Stephen Skirboll.
“We’re supporting neurosurgery training programs but also doing some task shifting, or task sharing,” Rosseau said. “This is a great example, neurosurgeons are taking one specific lifesaving procedure, a burr hole craniectomy, and teaching it to other specialty surgeons which will allow more lives to be saved.”
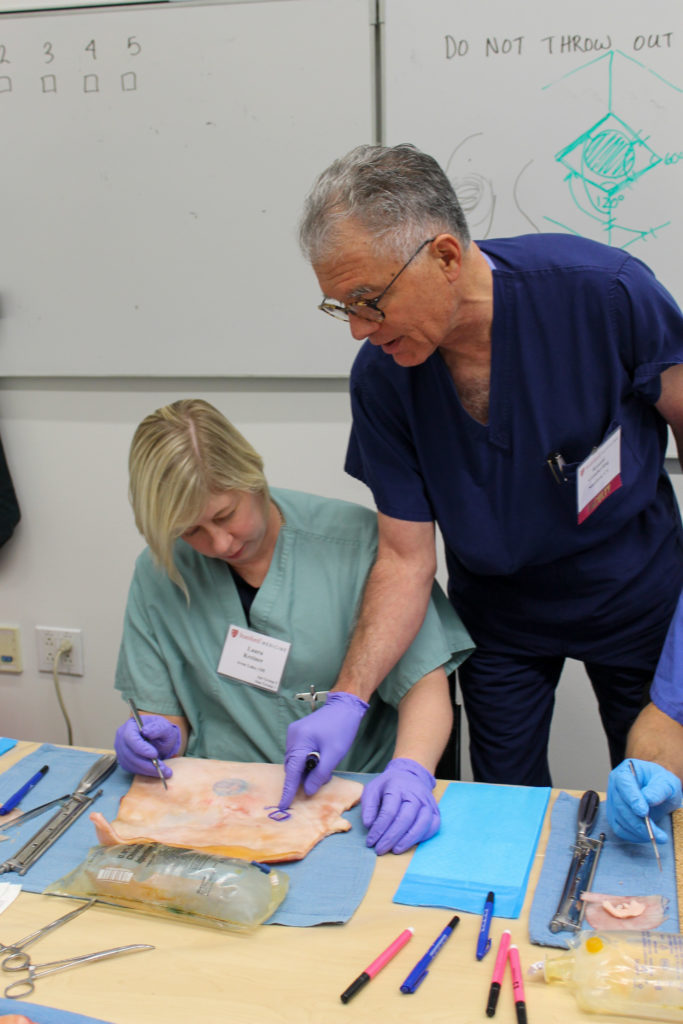
The first day is very busy with teaching sessions on tropical medicine and anesthesia practices by Susan Anderson from Stanford and Vanessa Moll from Zurich, Switzerland. Stanford plastic surgeon Peter Deptula co-taught the session on skin grafts with UCLA’s Ronald Gemberling. Stanford surgeons David Spain taught hernia repair, Raffi Avedian, Malcom DeBaun, and Nicholas Giori, as well as UCSF surgeons Rick Coughlin and Heather Roberts taught orthopedic skills. Hand surgeons Bobby Diaz from PAMF and Peter Johannet from Stanford taught repair of hand injuries.
The second day, participants learned OB-GYN procedures for low-resource settings from Drs. Kay Daniels, Amy Judy, Andrea Henkel, Sarah Peterson, Amy Huibonhoa, Caroline Bowker, Kimberly Harney, Gaea Moore, Paige Bates and Malte Renz.
“We have great faculty for this course,” Wren said. “And all of them volunteer their time to teach it.”
The course evolves every year based on student and faculty input. Wren is proud of her world class experienced global surgery faculty and diverse group of learners. Attendees are actively included. “I really encourage discussion because we all learn from each other,” Wren said.
And every year since its inception, the course has been oversubscribed because doctors, nurses, and PAs from all disciplines are inspired to follow Wren’s lead.