Published: 03/07/2022
Before Dr. Yvonne Maldonado became a leading researcher and communicator in the effort to vaccinate children against COVID-19, she devoted much of her career to combating childhood polio and HIV around the globe.
By Jamie Hansen

While Dr. Maldonado has recently received a great deal of recent U.S. media coverage for her efforts on COVID-19, it is her work alongside communities in Mexico and Sub-Saharan Africa that has defined much of her career. In our interconnected world, she says, it’s critical to work alongside communities in the global south to empower and support their public health efforts as a way to ensure the health security not just of those communities, but the entire world.
We sat down to discuss the need for a global, culturally responsive approach to combating childhood infectious disease with Maldonado, who is a senior fellow at the Stanford Center for Innovation in Global Health, Senior Associate Dean of Faculty Development and Diversity at Stanford’s School of Medicine, and Taube Professor of Global Health and Infectious Diseases.
Before this pandemic, you spent your career fighting two devastating illnesses that affect children, polio and HIV. How did childhood infectious disease become the target of your work?
Two key things that happened at the beginning of my career helped me focus on global child health. First, while working at the Centers for Disease Control (CDC) in the Epidemic Intelligence Service in the 1980s, I did a lot of work around HIV, its natural history, epidemiology, and prevention. At the time, we really didn’t understand how HIV impacted children and pregnant women. So when I came to Stanford in 1988, I set up the first HIV program for children and developed the HIV clinic. With funding from the CDC and the state health department, I set up a long-term epidemiological study of children in Northern California with HIV in partnership with UCSF and Children’s Hospital Oakland.
At the same time, in 1988, the World Health Assembly declared they were going to work to eradicate polio. I already knew that I loved working in prevention and child health because, I think, it’s the best way you can affect a life’s course. Obviously, maternal health is critical as well, but anything to do with young lives and vaccines struck me as the low-hanging fruit because we knew vaccine-preventable diseases accounted for a large share of child deaths around the world.
I saw an opportunity to vaccinate children and eliminate a whole lot of deaths. So, when I came to Stanford that same year, I chose to focus on polio. I still have a polio lab these many years later, and conduct National Institutes of Health-funded research to study how such diseases get transmitted, especially in developing settings, and how vaccine strategies to reach the hardest to reach children can help eliminate them. Polio is proof of our ability to eliminate a disease through vaccines.
I feel like the work that I’ve done has really been kind of bookended by these two viruses, polio and HIV. We’ve made a lot of progress in both, but they’ve also shown us how infectious disease can persist in children if we are not vigilant.

How has the pandemic impacted this progress in the fight against polio and other vaccine-preventable childhood diseases?
It was really heartbreaking to see recently the case of polio in Malawi, when we know that up until last year, in the midst of this intense, terrifying pandemic, there were only five cases of wild polio in the world, and in 2020, the Africa region was declared polio-free. I’m hopeful Africa can keep that designation because it appears this case in Malawi was an importation, a Pakistani strain, last found in 2019.
This case highlights how we are facing heightened disease transmission risks because of a lack of simple access to immunizations. We now may see not only polio, but also HPV rates go up. We’ve seen that the routine services we were able to provide pre-pandemic, even in the hardest hit countries in the world, are really crumbling.
The reduction in routine childhood vaccinations during the pandemic was about 7 percent below normal, which is tragic, but only about half that was originally projected. Still, it will take the world a decade or more to return to normal vaccination levels.
Child health has suffered from this pandemic in ways that I think we won’t see for 10, 20, or even many years beyond because we’ve really affected child development all around the world.

How did your work on polio and HIV help prepare you for your work on COVID-19?
COVID-19 is an extension of all of the things we’ve done before. It’s a reminder that we need to constantly keep on guard and make sure that we are protecting all of our populations — because when we don’t, there are always unintended consequences.
The last big pandemic in 1918 happened because of a confluence of many of the same factors that led to COVID-19: people from around the globe gathering together, allowing the ability of organisms to spill over into humans. Now, we can be anywhere in the world in 24 hours. So this is going to keep happening. We’ve opened the gate.
How do we move forward and learn from this pandemic?
They say eternal vigilance is the price of freedom. Well, eternal vigilance is also the price of a long life. That is true for every child in the world, not just those who live in poor countries. If we think about what we’ve gone through in this country in the last two years, I don’t think we can imagine what the global south has faced. We must learn lessons from this in terms of collaborating not only at an individual or an academic level, but at a political, a geopolitical level to ensure that children all around the world have access to care.
One lesson that we’ve learned the hard way is that lack of access in any part of the world means lack of access in the whole world. This point has been driven home, in a very striking way, with COVID. And we know that health for children in the long-term means better economic health and better security, both at a national and international level. So, I think, there’s no better place to start than working with mothers and kids and families.

COVID-19 has laid bare the dangers of vaccine hesitancy and made the term a household phrase — but vaccine hesitancy is nothing new. Has COVID-19 revealed new insights about this phenomenon, how it manifests itself in different cultures around the globe, and how it can be overcome going forward?
I’m a member of Lancet Commission on Vaccine Refusal, Acceptance, and Demand, a group that was actually commissioned before COVID-19 that has since turned its focus to the pandemic. As you note, the basic principles of vaccine hesitancy have always been there, but with COVID-19, it hit us hard and it hit us below the belt.
Most of us who work with vaccines knew that this hesitancy issue had been around for a long time, that how dangerous it was. But in the early days, we thought it was really an issue of higher income countries because in lower and lower middle income countries, the primary concerns were lack of access and education.
Now, as the world has seen greater vaccine access and development, so it has seen the expansion of social media platforms that provide access to misinformation — such that we started to see hesitancy in all countries even before COVID-19.
A big part of the problem was lack of community engagement and lack of partnerships, which fuels bad actors who are responsible for an incredibly tragic and fatal stream of misinformation. As the researcher or policymaker, you can’t come in as an expert and force things on them, because you are not an expert in what a community or region may be facing. Rather, it’s a matter of partnering with smart, capable people who really just need good partnerships to be able to build out their messages in a way that’s culturally appropriate.
We saw this with polio. The success of polio eradication efforts was due to global health researchers and policy makers, such as those at UNICEF, working side by side, shoulder to shoulder with community advocates and partners.
When we use this kind of approach, I think there can be hope.
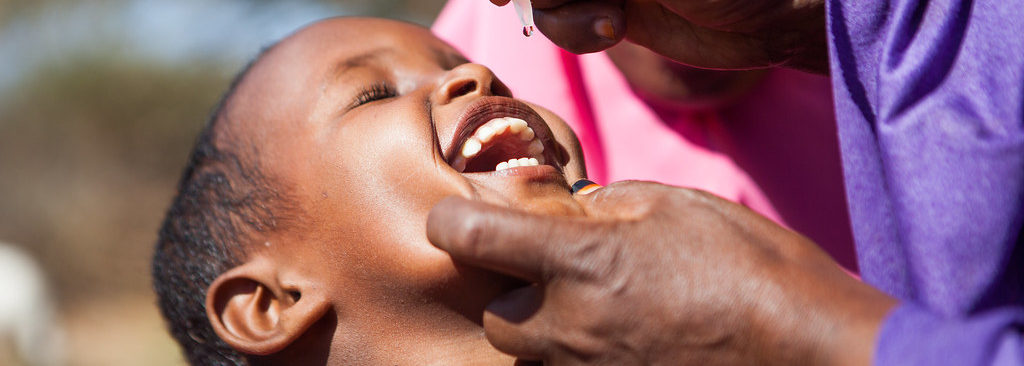
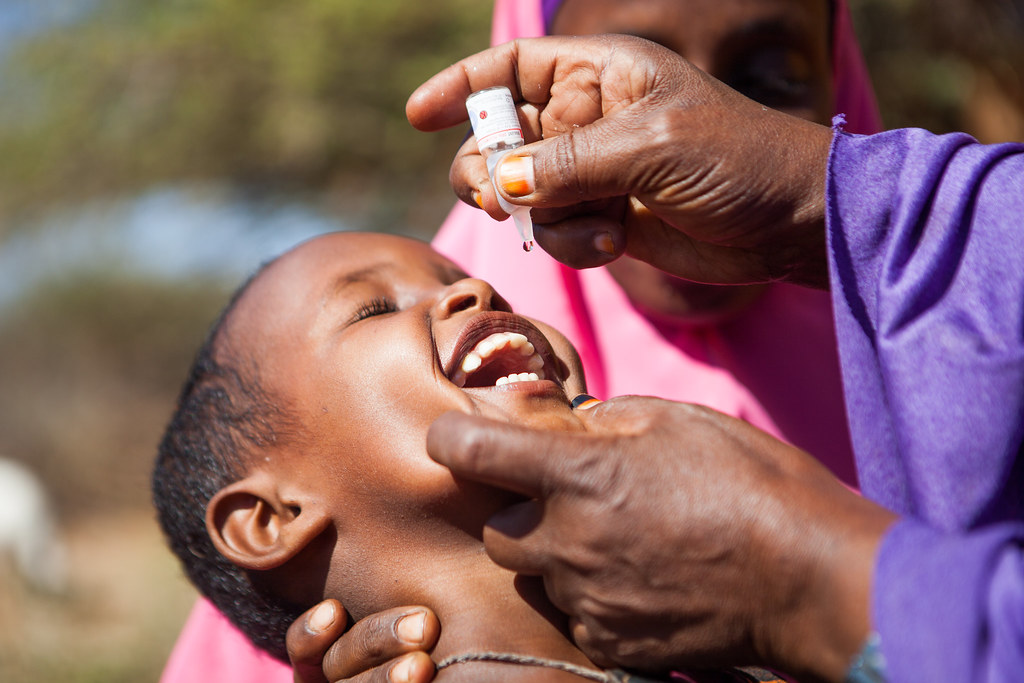
Header Photo: UNICEF Ethiopia, 2013