Published: 03/07/2022
By Jamie Hansen
Early in the pandemic, unequal access to medical technology and equipment was felt around the globe. But perhaps an even more critical need than technology was knowledge — specifically, an understanding of how to provide oxygen therapy and critical care.
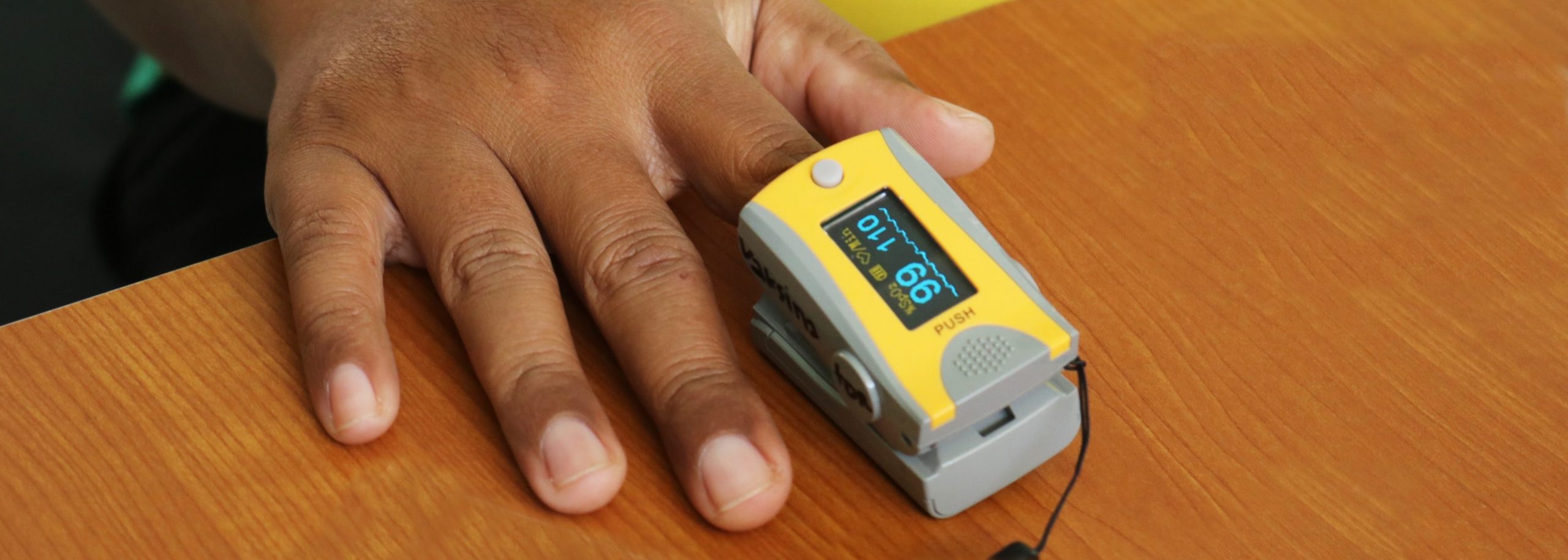
In rural and low-resource areas with few medical specialists, providers suddenly needed to know life-saving skills such as using pulse oximetry to monitor oxygen levels and how to put a critically-ill patient on a ventilator.
“Empowering the workers with knowledge is what matters before we think of having equipment. Because you can have equipment that you don’t know how to use,” said Dr. Papytcho Ntambwe, an anesthesiologist at Livingstone Central Hospital in Zambia.
“Empowering the workers with knowledge is what matters before we think of having equipment. Because you can have equipment that we don’t know how to use.”
Dr. Payptcho Ntambwe, Livingstone Central Hospital, Zambia
That’s why, when his colleague Dr. Ana Crawford, founder of Stanford Anesthesia and Critical Care Department’s Division of Global Health Equity, invited him to participate in a virtual panel to help mentor colleagues around the world in these skills, he eagerly accepted. Ntambwe and colleagues from many other African and Latin American countries joined Dr. Crawford to provide a series of 12 webinars offering life-saving skills and training in oxygen therapy to frontline workers around the world.

Dr. Ana Crawford founded the Division of Global Health Equity within the Department of Anesthesiology, Perioperative and Pain Medicine. She is also a clinical associate professor of anesthesiology, perioperative and pain medicine and a Global Health Faculty Fellow at the Stanford Center for Innovation in Global Health.
The webinars, combined with an interactive online learning platform that Crawford developed, have now reached 8,200 learners from 145 countries and inspired the creation of 10 learning hubs across the world.
Crawford and her colleagues, like Ntambwe, believe this model, born of necessity during the pandemic, could revolutionize the ability to provide high-quality mentorship and training to hard-to-reach places in the world.
The project began when Dr. Michele Barry, Director of the Center for Innovation in Global Health, received a request from the World Bank for help setting up virtual COVID-19 training programs for medical providers. Barry reached out to Crawford, a global health faculty fellow at the center who had recently developed an online training program for an anesthesia program she’d been involved with in Rwanda.
Crawford first sought to connect The World Bank with large organizations that might be able to assist, but found that their size made them slow to respond. So, she decided to build the program herself.
“I was kind of a speed boat as opposed to the larger barges,” she said.
Crawford had no technical experience aside from her self-taught work developing an online learning platform in Rwanda. However, a friend had told her about a user-friendly platform, and she dove in. She created The Global Anesthesia and Critical Care Learning Resource Center (LRC).
The LRC is an open-access virtual platform designed to support self-directed learning through quizzes, case studies and exercises, video demonstrations, clinical decision-making tools, peer-reviewed resources, and more.

Next, she developed a series of webinars in collaboration with Assist International, an organization that designs and implements humanitarian programs that build capacity, develop opportunities, and save lives around the world. The webinars were meant to provide real-time mentorship and expertise to healthcare providers around the world on topics such as personal protective equipment, ventilation, isolation in hospitals, and mechanical ventilation for the critically-ill.
“For our webinars, I knew we needed a mix of panelists from high- and low- resource settings so we could have a robust discussion and learn from one another,” she said.
“For our webinars, I knew we needed a mix of panelists from high- and low-resource settings so we could have a robust discussion and learn from one another.”
Dr. Ana Crawford, founder of the Stanford Division of Global Health Equity within the Department of Anesthesiology, Perioperative and Pain Medicine
So, she reached out to friends and colleagues in Africa and Latin America with whom she’d developed close relationships over the course of 12 years working in Global Health.
Dr. Alhassan Datti Mohammed, an anesthesiologist from Nigeria, had been collaborating with Crawford since 2018 and eagerly accepted the opportunity to help educate others around the globe. “We wanted to show there are always ways to do the right thing with what you have, no matter the setting,” he said. “Even if we don’t all have the same resources, there are things you can do.”
Panelists like Mohammed and Ntambwe then helped spread the word about the webinars through their networks, ensuring a large and diverse turnout.
Following the success of the webinars, Crawford and Assist International worked with partners like Mohammed and Ntambwe to create 10 learning hubs serving various regions around the global south. These hubs offered tele-mentoring programs led by local clinical experts as well as an online community organized over WhatsApp where participants can ask questions, crowd-source solutions to local challenges, and build lasting connections with other providers.

“Our remote delivery of sessions, in combination with active social media groups, has allowed us to reach thousands of nurses and doctors that might not otherwise have had opportunities to mentorship and clinical educational opportunities,” said Alana Changoor, program associate for global health at Assist International. “The result has been the creation of a global network of providers, supporting one another during these trying times!”
Dr. Rodrigo Rubio, an anesthesiologist at a leading hospital in Mexico, partnered with Dr. Fredy Ariza Cadena of the Fundación Valle del Lili in Columbia to organize the Latin American hub. They have reached healthcare providers across almost all Spanish-speaking countries in Latin America, he said.
“I love the virtual model, and I hope it stays,” he said, adding that the virtual approach made the program much more accessible to professionals in rural areas who find it hard to travel to cities to receive professional development.
Now, Crawford hopes to expand the program beyond its COVID-19 uses to provide training and support in other areas—primarily, critical care. Already, she has hosted a 2-part series on addressing sepsis and shock.
Ntambwe agreed: “When I meet colleagues asking me when the next series will start, I realize how important the program was,” he said. “I wish to see another similar one taking place and covering other topics.”
Cover photo courtesy of USAID Tanzania