Published: 12/17/2021
As a doctor, epidemiologist, and award-winning journalist, Seema Yasmin has seen how medical contagion is almost always accompanied by viral misinformation. The medical community has often ignored this interconnection, she says — at the cost of health equity. Recently, a proliferation of medical misinformation created vaccine hesitancy that has hampered global COVID-19 vaccination efforts.
By Jamie Hansen

Dr. Yasmin is leading the fight against medical misinformation and toward information equity on numerous fronts. Her new book, Viral BS: Medical Myths and Why We Fall for Them, dissects medical myths to understand why they spread and why we believe what we believe. A forthcoming book, “What the Fact: Finding Truth in All the Noise” will help young adults distinguish fact from fiction in the hope of building a more media-literate generation. As director of the Stanford Health Communication Initiative, she works to increase equity in health care by improving the way doctors and scientists communicate with patients, the press, and the general public. Most recently, she has been appointed to a new committee convened by the National Academies of Sciences, Engineering, and Medicine (NASEM) to address inaccurate and misleading information about biological threats.
We sat down with Dr. Yasmin to discuss how equitable access to information can help achieve vaccine equity and improve health worldwide.
There’s a lot of talk right now about vaccine equity, and you contend that information equity is critical to achieving this. How does the way we deliver information impact public health outcomes—and what we can expect in the future?
Really early in the pandemic, I was on a panel for news leaders in the Bay Area. My focus was very much on the impacts of misinformation and disinformation. An editor from a Central American indigenous language news organization was like, “Talking about misinformation and disinformation isn’t very helpful when we’re just not getting any information about is (COVID-19) real, what is it, and how does it spread.”
Communities are not monolithic and they have very different informational needs. We tend to make assumptions in public health, like I did on that panel. We assume we know what people need, crafting messages and information without doing the groundwork to assess what information might actually be helpful to them. It’s a very paternalistic, top-down approach.
I teach many case studies about this very phenomenon, the knowledge deficit model of science communication, which is: “ I’m the physician, I’m the scientist, there’s a knowledge gap. I can bridge it just by translating this technical information into language that’s suitable for you.” And it so misses the mark very, very many times — even with our best intentions — and it backfires too, because we are not assessing first what our audiences need.
How does an individual’s access to information impact health – particularly during an epidemic or pandemic?
I’ve been mapping the presence of news deserts — places without local newspapers, radio, television, or broadband news. We’ve found significant evidence that living in a news desert is bad for democracy and, as it turns out, it might also bad for your health. In the absence of trusted information, people are more vulnerable to medical myths.
For instance, our preliminary analysis has found that if you live in a news desert, you are less likely to be vaccinated against COVID-19. We’re interested in looking at more individual and public health metrics to understand the dynamic between people’s access to information and how vulnerable they are to misinformation and disinformation, health hoaxes, and medical myths — and then, how that impacts their health.
And we’ve already seen indications of this during the pandemic. Several papers out of the University of Chicago looked not only at where people got their news, but exactly which anchor on which network informed their approach to the pandemic. Researchers found a correlation between which news anchor people watched, the anchor’s stance on the pandemic, and how likely individuals were to follow public health advice and even get sick from Covid-19.
What have you learned from your family of immigrants about how their experiences might impact their willingness to trust the medical and media establishment?
I cringe when I note myself sending BBC or New York Times articles that have really solid reporting around the vaccine to my family, when I understand that my family has a particular experience of witnessing their faith being misreported and misrepresented in the New York Times, or they have a particular critique of, say, the BBC’s reporting on Israel and Palestine. They might choose to believe they’re reading stellar vaccine reporting, but they might also think, even subconsciously, “How can I trust this, given what else I know about how these news organizations report on my faith and my community?”
We grow up excluded or misrepresented in these news outlets, which are not entirely terrible — a lot of what they do is fantastic, and so useful in the pandemic. But how do we balance that and how do we build trust in news and science?
It’s a problem of authority. When the Ebola epidemic began in 2014, I was a newspaper reporter for the Dallas Morning News. I remember interviewing a Liberian immigrant who was fundraising to send money back home. I naively assumed he was raising money for medical supplies. In fact, he wanted to buy radio air time so that his family would hear a trusted voice saying Ebola was real, to convince them to leave Monrovia and go to the countryside. There was such a distrust of the government, and of course there would be, given Liberia’s very recent history with civil wars and the way the government handled the press.
Again, it’s a problem of a paternalistic approach to communication. And I think it’s a problem of not understanding the informational needs of different groups.
How can we do better?
I think we have to acknowledge that the problem of information inequity exists in the first place.
In journalism, we’re beginning to see the start of some process of atonement, or at least acknowledgement. National Geographic has apologized for its reporting of indigenous people as inferior to white people, The New York Times is apologizing for some of its reporting on black women who became addicted to crack in the ’80s and ’90s, and the The L.A. Times has apologized for its editorials that endorsed internment of Japanese Americans.
What has the medical world done to acknowledge or atone for past and current racism and ableism? The Tuskegee Experiment comes up a lot, obviously, in the conversation around vaccine trust and distrust among Black Americans. And while Bill Clinton apologized to survivors of that clinical trial, decades later, that conversation can sometimes disregard modern day medical racism. If the same person that dismissed your pain, the same person that dismissed the concerns of a black woman in labor and who represents an establishment that uses racist algorithms in clinical decision-making, is the person asking you to trust them to get vaccinated, how do we expect that conversation to go?
You’ve critiqued the idea of returning to normal after the pandemic, pointing out that “normal” created the conditions for the COVID-19 pandemic in the first place. In light of what we’ve just talked about, how can we start building a better system that is less paternalistic, that gains trust?
I think it needs to be shaken up in really drastic ways.
We need to consider what we hope or think the policy and public implications of our research might be — for example, think about which communities we hope to impact. And then, instead of assuming that we know best how to serve those communities, we bring in and engage those community members in the research process. I think that’s one of the ways.
We need to ask questions and listen. While we shouldn’t necessarily assume medical knowledge among laypeople, we should assume cultural capital, cultural knowledge.
As much as we might be experts in case control studies or a particular pathogen, community members are experts in their lives and their ways of doing things.

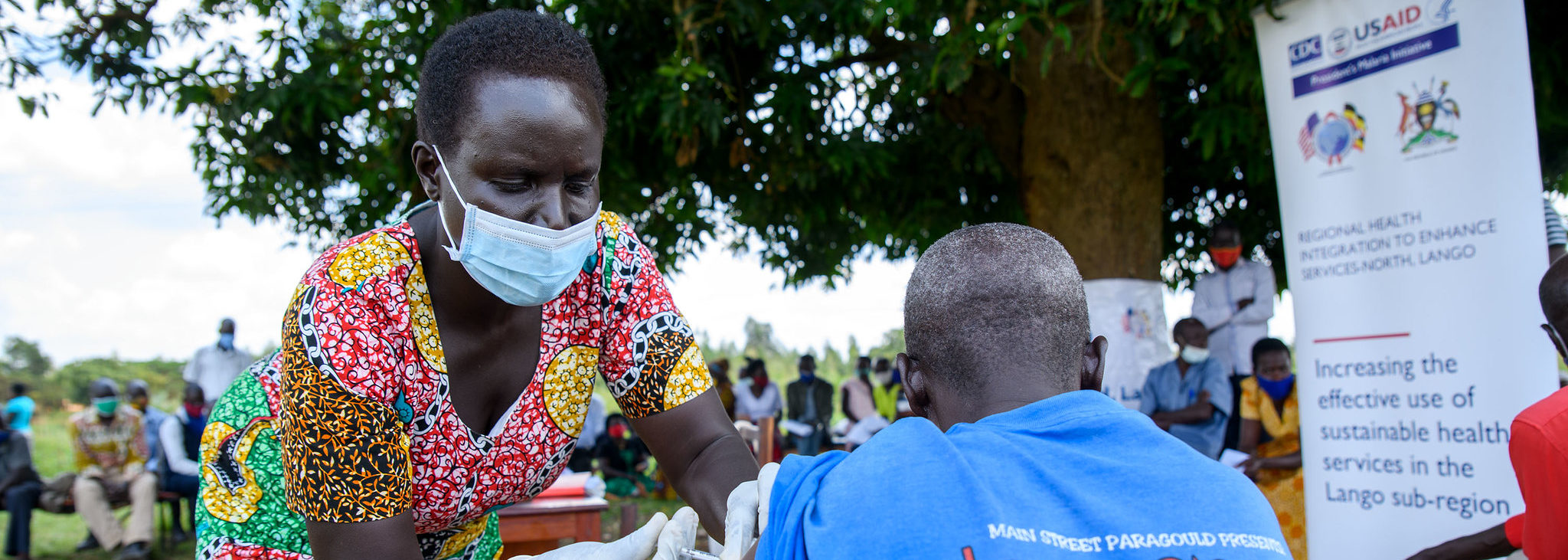
Header Photo by USAID/Uganda