Published: 03/16/2022
By Jamie Hansen
Helping Midwives at the Border Save Lives
A collaboration between Stanford doctors and Tijuana midwives that began in response to the twin challenges of the border crisis and the pandemic has proven an effective model for equipping midwives serving refugees with life-saving skills. Its value could last well beyond the pandemic and help midwives safely deliver many more babies outside the hospital, said lead midwife Ximena Rojas.
A small and dedicated team of about eight midwives had been serving refugee mothers at the border for years, but when COVID-19 struck, overwhelmed hospitals would no longer admit refugees. The midwives saw a nearly tripling in the demand for their services at the height of the pandemic.
“We used to be able to advocate for a family that was high-risk to be seen in a local hospital, but when COVID-19 arrived, we had to start from scratch.”
Ximena Rojas
“We were delivering 2-3 babies every 24 hours and barely had time to eat or sleep,” recalled Rojas, leader of the Refugee Health Alliance which supports maternal and child refugee health in Tijuana. “We used to be able to advocate for a family that was high-risk to be seen in a local hospital, but when COVID-19 arrived, we had to start from scratch.”
“The midwives started seeing very clearly a higher percent of babies having issues, with breathing problems being most common,” Xinshu She, MD, a Global Health Faculty Fellow and pediatrician at Stanford. “Most of these women were experts in maternal care, but they weren’t necessarily used to dealing with babies that didn’t breathe or looked blue.”
She added that addressing breathing issues in the first 5-10 minutes of a baby’s life is crucial to their survival.
The midwives sought help and training in how to resuscitate newborns through Families at the Border, a network of Stanford refugee health advocates including pediatricians, emergency medicine doctors, staff, community members, and students created in 2019 by Stanford Drs. Lisa Chamberlain and Kay Daniels in response to reports of child deaths at the border.
The group, led by Maggi Smeal, mobilized to design four virtual training sessions to help 18 midwives learn to recognize and address the signs of respiratory distress in newborns.

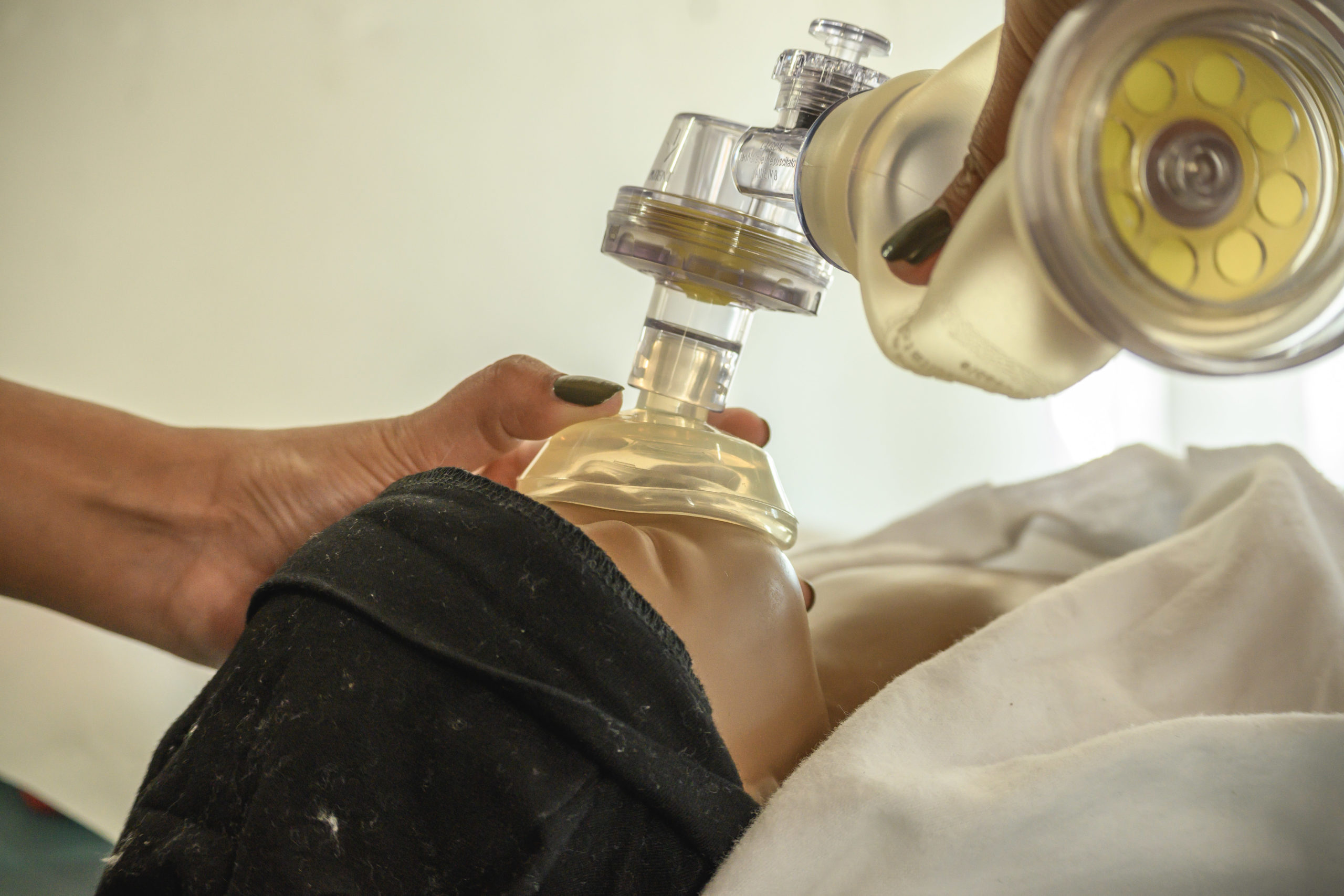
Laerdal Global Health, a company specializing in resuscitation training equipment, donated five “helping babies breathe” kits for the training. They later donated NeoNatalie mannequin/simulators used in tandem with the Helping Babies Breathe Curriculum from the American Academy of Pediatrics, which is proven to reduce mortality in newborns by 40 percent. Experts like She, who is fluent in Spanish and has led similar efforts in Haiti, provided the training.
After the training, the midwives reported feeling supported and confident in their ability to help an infant in distress.

Rojas said the experience proved a great training model, which she now employs whenever a new midwife joins the team. “Some of our volunteers have just graduated, and while they have the training, they don’t have all the skills and practice,” she said. “The mannequins, and the expertise of the Stanford experts, help a lot.”
She added that the experience has helped strengthen her team’s ability to respond to emergencies and expanded their capacity to safely deliver babies outside the hospital.
And when C-Section rates at local hospitals are as high as 95 percent, the ability to deliver more babies outside of that setting can be therapeutic for all involved, she said: “For families with so many layers of trauma, we believe that delivering a health baby together is a way of healing that trauma.”
Interested to learn more?
Tune in to the team’s presentation, ‘Just in time’ training using virtual simulation, at the Consortium of Universities for Global Health Conference, Thursday, March 31. The team includes She, Rojas, Chandani DeZure, Sunniya K Basravi, Rishi Mediratta, Caroline Toney-Noland, Kay Daniels, and Maggi Smeal.